The iliotibial band (ITB) a.k.a. iliotibial tract is a thick fascia on the lateral aspect of the knee as well as hip.
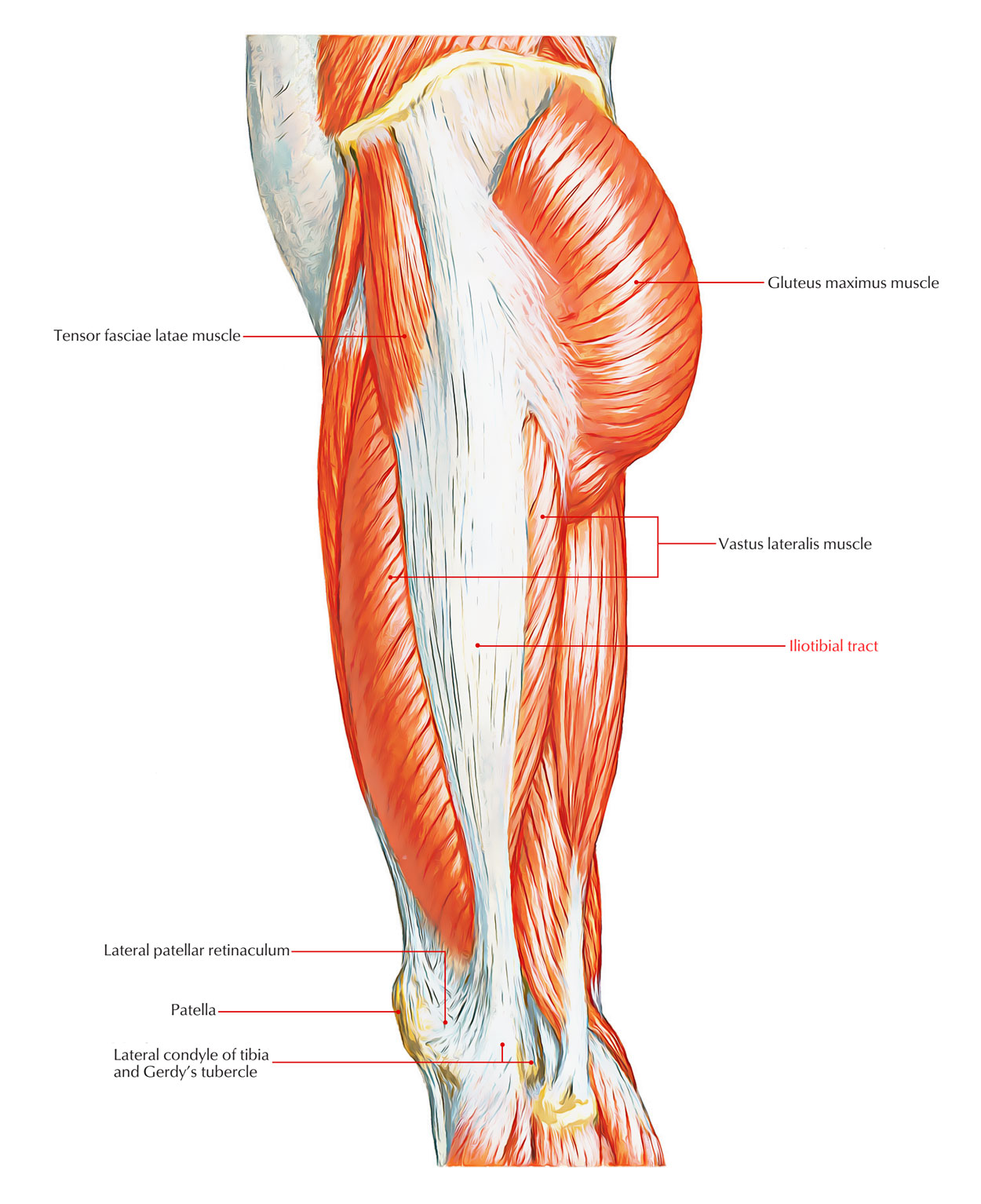
Iliotibial Band
Attachments
1. The gluteus maximus and tensor fascia lata generally were believed to be the proximal genesis of the ITB.
2. The gluteus medius also has direct and also indirect contributions to the ITB.
3. Proximal connection consists of the iliac tubercle or iliac crest.
4. In the distal thigh, the ITB connects to the linea aspera as well as the upper edge of the lateral femoral epicondyle.
5. After passing over the lateral femoral epicondyle, it splits into two parts:
- The iliotibial pathway of the distal ITB connects to Gerdy’s tubercle of the anterolateral proximal tibia.
- The iliopatellar band of the ITB has aponeurotic attachments to the patella as well as the vastus lateralis.
- Other distal connections consist of the biceps femoris, the lateral patellar retinaculum, and the patellar tendon.
6. An anatomic pouch can be discovered under the posterior iliotibial band at the level of the lateral femoral epicondyle.
7. Others have actually reported that an extremely innervated fat pad is located over the lateral femoral epicondyle.
Function
- It also permits the tensor fasciae latae and gluteus maximus muscles support and support of the knee while standing, strolling, running and biking and so on.
- Functionally, the iliotibial tract extends the tensor fasciae latae muscle enabling it to work as an abductor, medial rotator and flexor of the thigh.
Iliotibial Band Syndrome
Iliotibial band syndrome (ITBS) or iliotibial band friction syndrome is an overuse injury usually describing lateral knee pain as a result of impingement of the distal ITB over the lateral femoral epicondyle. Although the anatomic pain generator might not be totally understood, pain at the distal element of the ITB is believed to be triggered by the fibers of the ITB passing over the lateral femoral epicondyle with knee flexion anti extension.
Less typically, ITBS might describe hip pain connected with movement of the ITB throughout the greater trochanter. The presumed pain generator in ITBS is as questionable as the anatomy over the lateral epicondyle. It has actually been postulated to be bursitis, synovitis or inflammation of the fat pad, posterior fibers of the ITB, or periosteum.
Symptoms
- Symptoms of ITBS happen usually at the lateral femoral epicondyle however might originate from the distal connection of the ITB at Gerdy tubercle on the tibia.
- ITBS is the most common reason for lateral knee pain in runners. People present with sharp or burning lateral knee pain that is exacerbated throughout repeated activity.
- This pain might radiate up into the lateral thigh or down to Gerdy tubercle. Runners typically explain a specific, reproducible time when the symptoms begin.
- Pain typically subsides after a run; nevertheless, in serious cases, consistent pain might trigger limitation in range.
- Runners also keep in mind more pain with downhill running because of the increased time invested in the impingement zone.
- Paradoxically, runners specify that faster running and running frequently do not produce pain.
- Quick running enables the professional athlete to invest more time in knee angles greater than 30 degrees. Bicyclists present with balanced, stabbing pain with pedaling.
- Particularly, they experience pain at the end of the down stroke or the start of the upstroke. Bicycle riders with incorrect saddle height and cleat position might experience greater symptoms.
- ITBS symptoms might also appear as a lateral hip snapping.
- An external or lateral snapping hip takes place as the ITB quickly passes anteriorly over the greater trochanter as the femur passes from extension to flexion.
- Professional athletes, especially dancers, in some cases experience an audible agonizing breeze on landing in bad turnout (reduced external rotation at the hip) and with extreme anterior pelvic tilt.
Treatment
If one is struggling with ITBS, the first thing one will have to do is stop running momentarily. However this does not suggest that a person ought to be totally inactive. ITBS is best treated with active healing, so even if not running, one ought to be doing specific workouts to reinforce weak locations and return on track rapidly. Both avoidance and treatment of ITBS originated from reinforcing the hip and gluteal muscles.
Inactive jobs and way of lives add to this weak point; however strength training is an easy method to eliminate it. If injury is current and reasonably minor, one need to be well better in 1- 2 weeks. Chronic, more severe cases might take longer, however do not anguish.
Dealing with the source of the issue will get one back to running ultimately, and one will be more powerful and more durable than one were prior to injury.
Physiotherapy Treatment
- Side Leg Raise.
- Clam Shell.
- Hip Thrust.
- Side Hip Bridge.
- Side Shuffle.
- Handgun Squat.
- Hip Walking.

 (56 votes, average: 4.81 out of 5)
(56 votes, average: 4.81 out of 5)