The menisci essential functions in preserving proper joint health, stability, as well as function. Every meniscus is thick as well as convex at its perimeter (the horns) however ends up being thin and also concave at its center. A larger area for the rounded femoral condyles along with the fairly flat tibia is offered through this contouring.
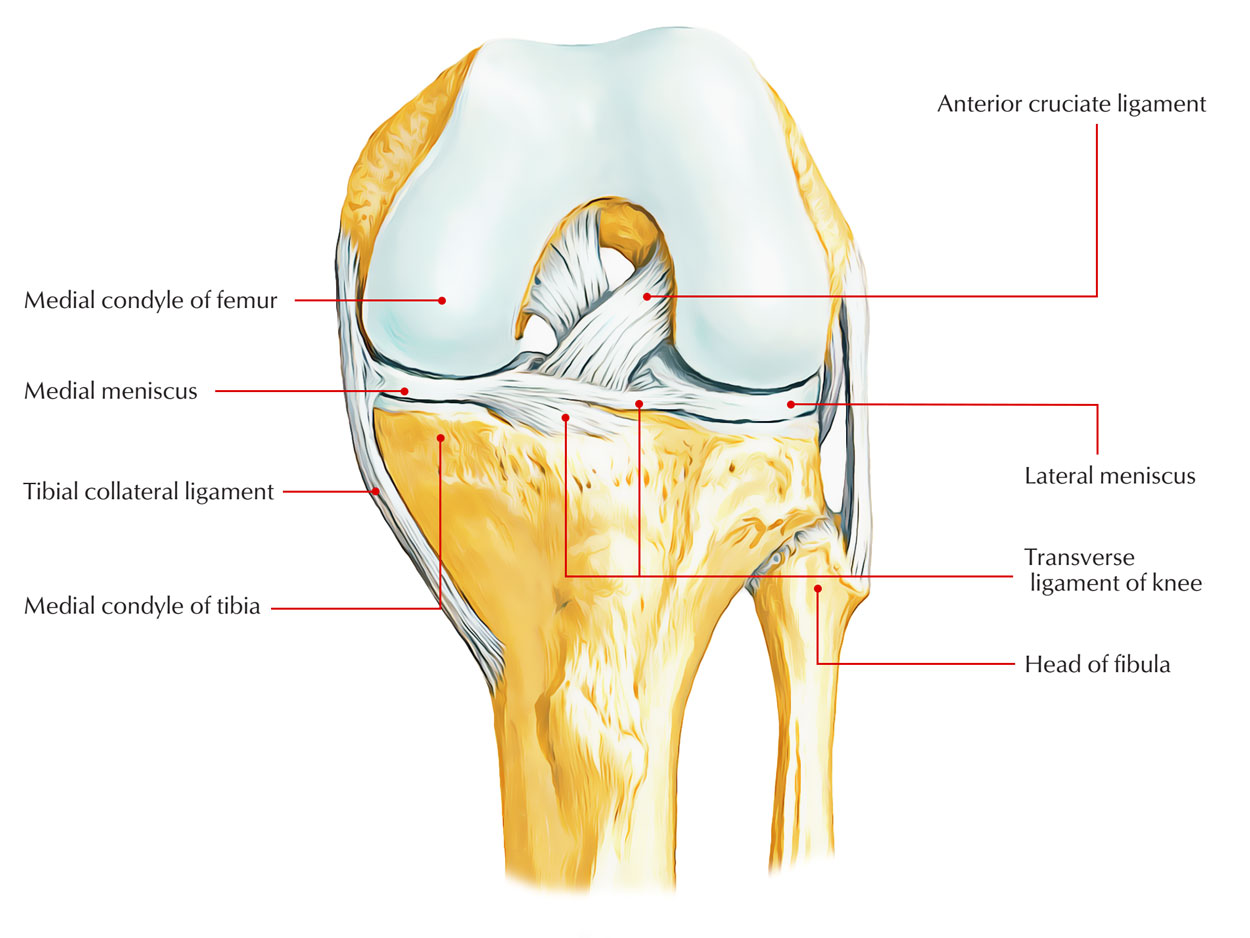
Medial meniscus
- The medial meniscus is less movable compared to the lateral meniscus. This reduced mobility, in conjunction with that the medial meniscus is larger posteriorly, is pointed out as the typical factor for the greater occurrence of tears inside the medial meniscus compared to inside the lateral meniscus.
- The semimembranosus muscle (through connections via the joint capsule) assists pull back the medial meniscus posteriorly, functioning to prevent entrapment and injury to the medial meniscus as the knee is bent. This is because of its steady links to the knee joint capsule and the medial collateral ligament.
Structure
Inside each region the structure and connections of meniscus vary and for that reason various surgical strategies are needed in order to accomplish anatomical restoration. Medial meniscus can be categorized into five anatomical regions.
Region 1
Region 1 includes the anterior root of the medial meniscus. The core of the anterior root of the medial meniscus is located conterminous to the superior element of the medial edge of the tibial tuberosity. In relation to arthroscopic sites, the anterior root of the medial meniscus is anterior to the pinnacle of medial tibial altitude and anterolateral to the edge of the articular cartilage of the medial tibial condyle.
Region 2
A particular is that within this region, the medial meniscus connects to the bone just with mcnisco-tibial ligament (coronary ligament). Region 2 consists of the antero-mcdial part of the medial meniscus. The superior edge of the medial meniscus in region 2a has no connections to surpivoting tissues; nevertheless, in region 2b the superior border of the medial meniscus is connected to the synovial tissue. This particular region might be split even more into two subzones: 2a (via anterior root connection to transverse ligament) and 2b (via transverse ligament to anterior border of medial collateral ligament). Rebuilding this ligament must be considered in cases of meniscal suturing
Region 3
Region 3 consists of the part of medial meniscus at the degree of medial collateral ligament (MCL). It is the only region where the whole part of the meniscus is connected to the joint capsule. This connection is determined in some research studies as a deep layer of the MCL or as a support of the joint capsule.
Region 4
Region 4 remains in essence the posterior horn of medial meniscus. In this region, the superior edge of the medial meniscus does not connect to the joint capsule. This particular ligament, together with the posterior joint capsule, forms the postero-medial femoral recess. Region 4 is an extremely unique pan of the medial meniscus. On the other hand, the inferior part connects to the tibia through the meniscotibial ligament (coronary ligament). Not just is it among the most regularly hurt one however also extremely technically requiring for any kind of suturing. Nevertheless, this might possibly have an impact on the mobility of the medial meniscus (especially with non-absorbable sutures), which subsequently might be responsible for bad long-lasting follow-up. For that really factor, a strictly anatomic medial meniscus (with restoration just of menisco-tibial connection) might need to be thought about.
Region 5
Region 5 is the posterior root of medial meniscus. The attachment of the posterior root of the medial meniscus lies posterior as well as lateral via the medial peak of medial tibial spine.
Function
The medial meniscus divides the tibia and femur to reduce the contact area in between the bones, and works as a shock absorber lowering the peak connection force experienced. It also disperse load throughout activity as well as minimizes friction in between the two bones to permit smooth movement in the knee.
Clinical Significance
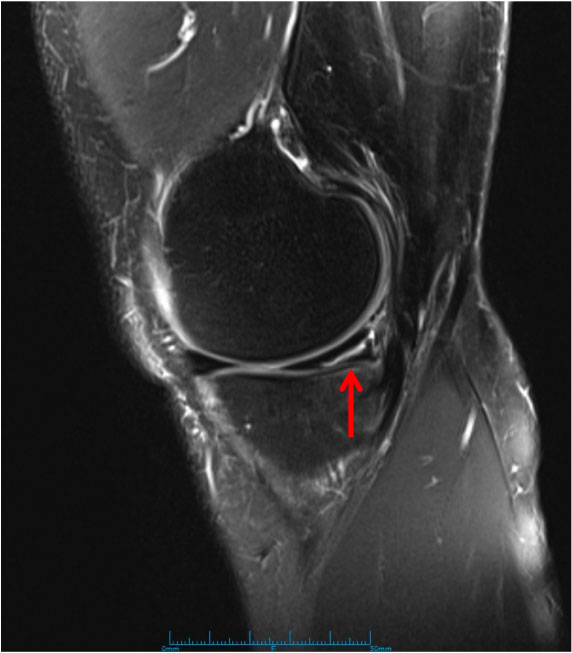
Medial Meniscus Tear
Medial Meniscus Tear A broken meniscus is a rip to the semicircular cartilage in the knee joint triggering pain on the within the knee. It is typically hurt through direct effect in contact sports or twisting however can also happen in older professional athletes through progressive deterioration. Treatment depends upon how bad the injury is and might need surgery.

 (48 votes, average: 4.85 out of 5)
(48 votes, average: 4.85 out of 5)