The conical shaped caudal end of the spinal cord lies on the rostral border of the second lumbar vertebra called the conus medullaris. A thin filament covered in pia and including glial cells, ependymal cells, and astrocytes arises out of the conus medullaris. This filament is referred to as die filum terminate internum. It expands via the conus medullaris and travels through the caudal end of the dural sac. At this level, a caudal thin elongation of the spinal dura, referred to as the coccygeal ligament (filum term inale externum) encompasses the filum terminale. The coccygeal ligament, along with the filum terminale in it, connects to the coccyx and, thus, supports the spinal cord together with the fluid-filled dural sac towards the caudal end of the vertebral canal.
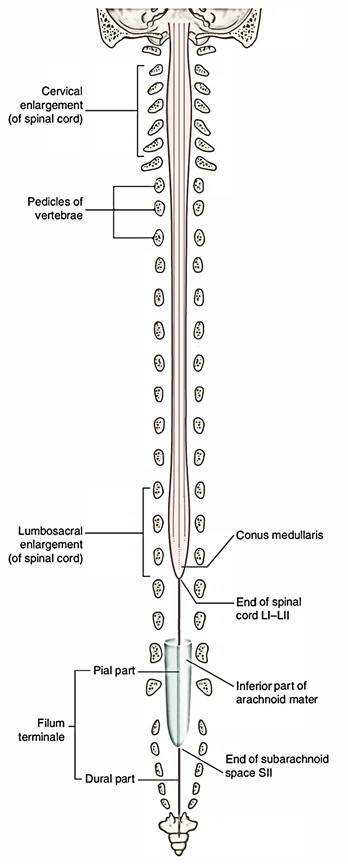
Filum Terminale
Insertion
The fragile thread for which this term is used is constant with the inferior tapered end of the conus medullaris. It is easily differentiated, by its silvery as well as sparkling appearance, by the numerous long nerve-roots (cauda equina) in the middle of which it is located. The filum terminale continues downwards within the sacral canal, and ultimately acquires connection to the periosteum on the posterior aspect of the coccyx. It is traditional to mention the filum as containing two parts, viz., the filum terminale internum along with the filum terminale externum, or the part inside as well as the part outside the tube of dura mater. It is around six inches long and downward to the level of the second sacral vertebra it is covered with the neighboring nerve-roots inside the dura mater. Under this point the dura mater is spread directly towards the surface of the filum terminale and is referred to as filum durae matris spinalis.
Structure and Parts
The filum terminale is a fragile strand of fibrous tissue, around 20 cm in length, continuing down via the apex of the conus medullaris. It is among the alterations of pia mater. It provides longitudinal support to the spinal cord and also contains two parts:
- The upper part, or filum terminale internum, is around 15 cm long and enters until the lower border of the second sacral vertebra. It is constant over with the pia mater and held within a tubular envelope of the dura mater. Furthermore, it is bordered by the nerves creating the cauda equina, where it can be easily identified by its bluish-white color.
- The lower part, or filum terminale externum, thoroughly follows the dura mater. It expands down via the top of the tubular sheath and is connected to the back of the first segment of the coccyx within a structure sometimes called as the coccygeal ligament.
Clinical Significance
Filar Lipoma
Lipoma of the filum terminale is created due to a developmental problem with mesodermal cell migration. Fatty filum terminale, also referred to as lipoma of the filum terminale or filar lipoma, is a comparatively general result on imaging of the lumbar spine, and in many cases is an occasional result of no clinical consideration. Nonetheless, in several patients it may be related to symptoms of tethered cord syndrome. In such cases it is usually related to a thickened filum and low lying conus.
Filum Terminale Syndrome
Tight filum terminale syndrome is created by incomplete convolution of the distal spinal cord at the time of embryogenesis. This results in progression of an unusually thickened filum terminale, which may be related to lipomas or cysts inside the filum. Tight filum terminale syndrome is always related to spinal cord tethering and an unusually located conus medullaris under L2-3 (normal range, L1-L2). Clinical symptoms are because of stretching of the spine with arising vascular deficiency at the level of the conus medullaris. These signs can occur at any age, may be indefinite, and include neurologic weakness, pain or dysesthesia, and bladder or bowel disorder.

 (48 votes, average: 4.69 out of 5)
(48 votes, average: 4.69 out of 5)