The two internal thoracic arteries can be differentiated as left and right. One on the either side of sternum and is located deep towards the anterior chest wall.
Origin
The initial part of the subclavian artery (lower surface) is the source of the internal thoracic artery situated around 2.5 cm over the medial end of the clavicle, opposite the origin of the thyrocervical trunk.
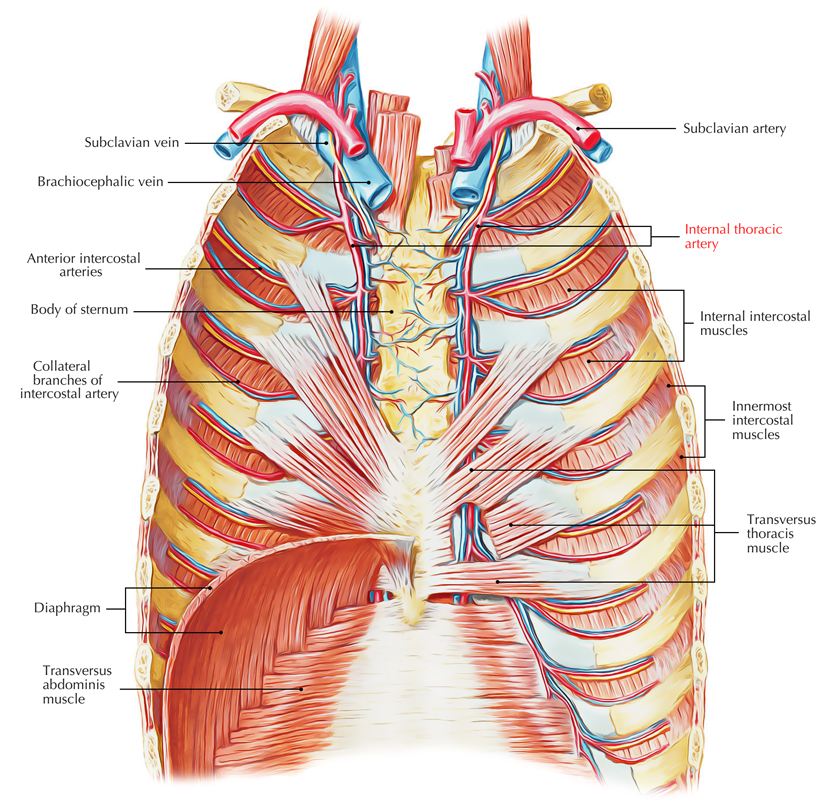
Internal Thoracic Artery
Course and Ending
The internal thoracic artery descends behind the medial end of the clavicle and upper 6 coastal cartilages, about 1 cm far from the lateral margin of the sternum. It finishes in the 6th intercostal space by breaking up into superior epigastric and musculophrenic arteries.
Connections
Anteriorly:
From above downwards, it’s related to:
- Medial end of the clavicle.
- Internal jugular vein.
- Brachiocephalic vein.
- Phrenic nerve.
- Pectoralis major.
- Upper 6 costal cartilages.
- External intercostal membranes.
- Internal intercostal muscles.
- Upper 6 intercostal nerves.
Posteriorly:
- Above the 2nd costal cartilage, it’s related to endothoracic fascia and pleura.
- Below the 2nd costal cartilage, it’s related to sternocostalis muscle, which intervenes between the artery and the endothoracic fascia and pleura.
The internal mammary artery is escorted by 2 venae comitantes, which unify in the level of 3rd costal cartilage to create the internal thoracic (mammary) vein, which runs upwards along the medial side of the artery to terminate into the brachiocephalic vein in the root of the neck.
Branches
- Pericardiophrenic artery: It originates in the root of the neck above the 1st costal cartilage, and descends together with phrenic nerve to the diaphragm. It supplies pericardium and pleura.
- Mediastinal branches: They’re small inconstant twigs, which supply connective tissue, thymus, and front of the pericardium.
- Anterior intercostal arteries: They’re 2 for every of the upper 6 intercostal spaces.
- Perforating branches: They accompany the anterior cutaneous branches of intercostal nerves. In females, the perforating branches of 2nd, 3rd, and 4th intercostal spaces are rather large and supply the breast.
- Superior epigastric artery: It runs downwards behind the 7th costal cartilage between the sternal and 1st costal slides of diaphragm to go into the rectus sheath where it stops by anastomosing with the inferior epigastric artery. It supplies anterior body wall from clavicle to the umbilicus.
- Musculophrenic artery: It runs downwards and laterally behind the 7th, 8th, and 9th costal cartilages, and supplies 2 anterior intercostal arteries to every of the 7th, 8th, and 9th intercostal spaces. It pierces the diaphragm near the 9th costal cartilage, to reach under surface. It supplies diaphragm and muscles of the anterior abdominal wall.
Clinical Significance
Function of Internal Mammary Artery in Treatment of Coronary Heart Diseases
The internal thoracic artery is occasionally utilized to take care of coronary heart disease. When the section of coronary artery is blocked by atherosclerosis, (largely), the diseased arterial section is circumvented by adding a graft. The graft most often utilized is taken from great saphenous vein of the leg. In certain patients, the myocardium is revascularized by marshalling the internal thoracic artery and joining its distal cut end to the coronary artery distal to the diseased section.
The Internal Mammary Artery Graft (Ima Graft)
The internal mammary artery graft (IMA graft) ispreferred over grafts from some other boats, because IMA graft continues long. Lately it’s been seen that internal mammary arteries are much less prone to develop atherosclerosis due to their histological peculiarity. The walls of these arteries include only elastic tissue and the cells of their endothelial lining secrete some compounds, which prevents atherosclerosis. The left internal mammary artery is favored over right internal mammary artery, because it’s simpler to access it.
Before the internal thoracic artery was utilized to be ligated in the 3rd intercostal space to be able to fortify the blood supply to the heart by redirecting blood from this artery to its pericardiophrenic branch. This process is now outdated.

 (63 votes, average: 4.59 out of 5)
(63 votes, average: 4.59 out of 5)