The Radius bone is a long horizontal bone present in the forearm and is also called The Radial Bone. It is one of the two bones of the forearm, the other being the ulna. The radius bone is shorter than the ulna and is prism-shaped long bone. The radius bone is homologous to the medial bone of the leg, tibia.
Radius Bone
What Type of Bone is The Radius?
There are five types of bones in the skeleton, these are flat bone, long bone, short bone, irregular bone, and sesamoid bone. All the major bones of the arms, including the radius bone are long bones. The function of long bone is to support the weight of the body and facilitate movement.
What Are The Various Parts of The Radius Bone?
The radius bone is made up of three parts, upper end, lower end and a shaft. Each part is discussed below separately.
Upper End
The upper end of the radius bone provides head, neck, and radial tuberosity. The head is disc shaped and articulates above along with the capitulum of humerus. Below the head is the neck, which is the constricted part. The radial tuberosity is just below the medial portion of the neck.
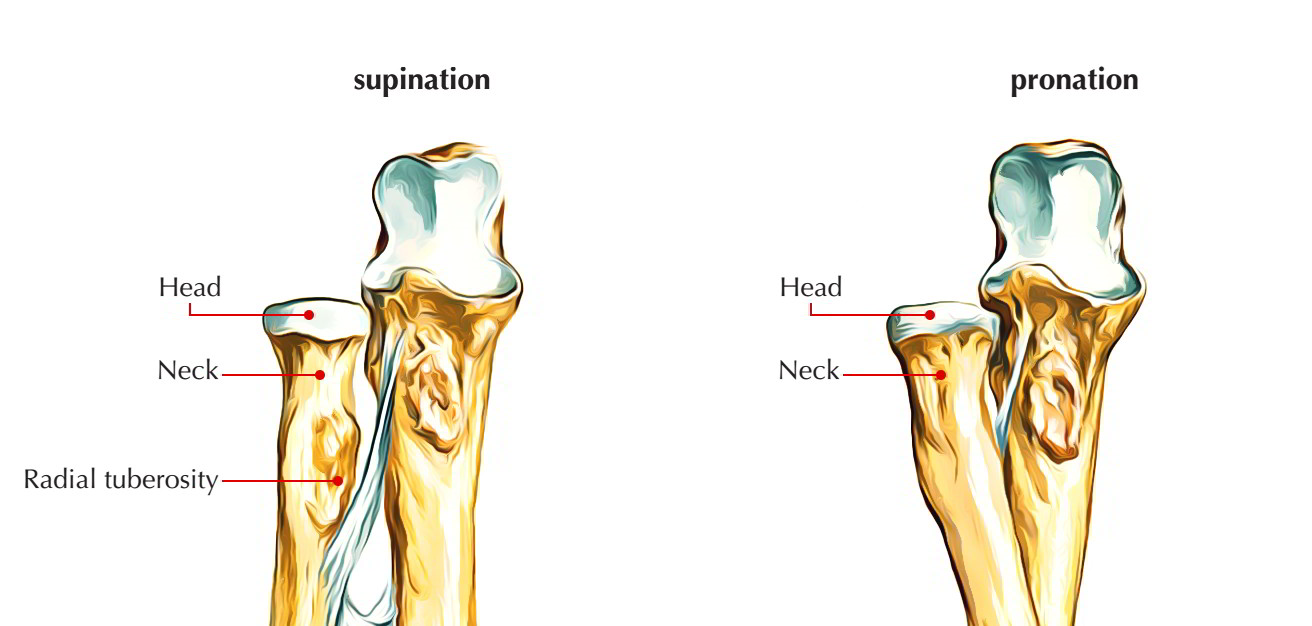
Upper End Radius Bone
Head
- The head of the radius bone is formed like a disc and in living it is covered by an articular hyaline cartilage.
- It articulates superiorly along with capitulum to create humero-radial articulation.
- The circumference of head is smooth and articulates medially along with the radial notch of ulna, rest of it is surrounded by the annular ligament.
Neck
- The neck of the radius bone is the constricted part just below the head and is embraced by the lower part of annular ligament.
- The quadrate ligament is connected to the medial side of the neck.
Radial tuberosity
- Biceps tendon is inserted to radial tuberosity’s rough, posterior part.
- A small synovial bursa covers its smooth anterior part and separates it from the biceps tendon.
Shaft
The long shaft of the radius bone provides a lateral convexity extending between the upper and lower ends. It broadens towards the distal end and is concave anteriorly in its distal part. Its sharpest interosseous border is located on the medial side.
The shaft of the radius bone has three borders and three surfaces.
Borders
Anterior border
- The anterior border of the shaft of the radius bone starts off below the anterolateral part of radial tuberosity and runs downwards and laterally to the styloid process.
- The upper part of this border is referred to as anterior oblique line and lower part forms the sharp lateral border of the anterior surface.
- Its anterior oblique line provides origin to radial head of flexor digitorum superficial (FDS).
Posterior border
- The posterior border of the shaft of the radius bone is well-defined only in its middle third of the shaft.
- Above it runs upwards and medially to the radial tuberosity and makes the posterior oblique line.
Medial (interosseous) border
- The medial border of the shaft of the radius bone is the sharpest border.
- It extends above up to radial tuberosity and below its lower part forms the posterior margin of the small triangular area on the medial side of the lower end of the bone.
- Interosseous membrane is connected to its lower three- fourth.
Surfaces
Anterior surface
- The anterior surface of the shaft of the radius bone is concave and is located between anterior and interosseous borders.
- Flexor pollicis longus emerges from its upper two-fourth.
- Pronator quadratus is inserted on its lower one-fourth.
- Nutrient foramen appears a little above the middle of this surface in its upper part. The nutrient canal is directed upwards. Nutrient artery for radius bone is a branch from anterior interosseous artery.
Posterior surface
- The posterior surface of the shaft of the radius bone is located between the interosseous and posterior borders.
- Abductor pollicis longus (APL) comes up from the middle one-third of this surface.
- Extensor pollicis brevis (EPB) comes up from lower part of this surface.
Lateral surface
- The lateral surface of the shaft of the radius bone is located between anterior and posterior borders.
- Supinator is inserted on the widened upper one-third of this surface.
- Pronator teres is inserted on the rough area in the most convex middle part of this surface.
Lower End
The lower end of the radius bone is the widest part and provides five surfaces. The lateral surface projects distally as the styloid process. The dorsal surface provides a palpable dorsal tubercle (Listers tubercle), which is limited medially by an oblique groove.
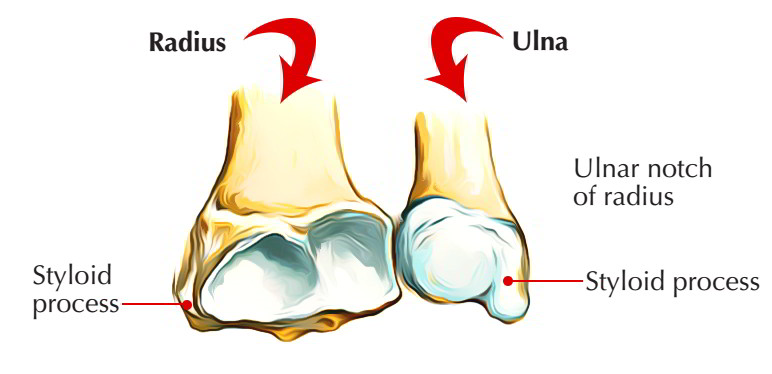
Lower End Radius Bone
The lower end is the widest portion of the bone and has five surfaces.
Anterior surface: The anterior surface of the lower end of the radius bone provides a thick ridge, which provides connection to palmar radio-carpal ligament of wrist joint.
Posterior surface: The posterior surface of the lower end of the radius bone provides the dorsal tubercle of Lister lateral to the groove for the tendon of extensor pollicis longus. It also provides grooves for other extensor tendons. The groove lateral to the Lister’s tubercle is traversed by tendons of extensor carpi radialis longus (ECRL) and extensor carpi radialis brevis (ECRB). Through the groove medial to groove for extensor pollicis longus passes tendons of extensor digitorum and extensor indicis.
Medial surface: The medial surface of the lower end of the radius bone provides the ulnar notch for articulation with the head of ulna. Articular disc of inferior radio-ulnar joint is connected to the lower margin of ulnar notch.
Lateral surface: The lateral surface of the lower end of the radius bone projects downward as the styloid process and is associated to tendons of adductor pollicis longus and extensor pollicis brevis. The brachioradialis is inserted to the base of styloid process and radial collateral ligament of wrist joint is connected to the tip of styloid process.
Inferior surface: The inferior (distal) surface of the lower end of the radius bone provides a lateral triangular area for articulation along with the scaphoid and a medial quadrangular area for articulation with the lateral components of the lunate.
What is the Anatomical Position of the Radius Bone?
The side of the radius bone can be identified by keeping the bone vertically in such a manner that:
- The narrow disc-shaped end (head) is directed upwards.
- The sharpest border (interosseous border) of the shaft is kept medially.
- The styloid process at the lower end is directed laterally and prominent tubercle (Listers tubercle) at lower end faces dorsally.
- The convexity of shaft faces laterally, and concave anterior surface of shaft faces anteriorly.
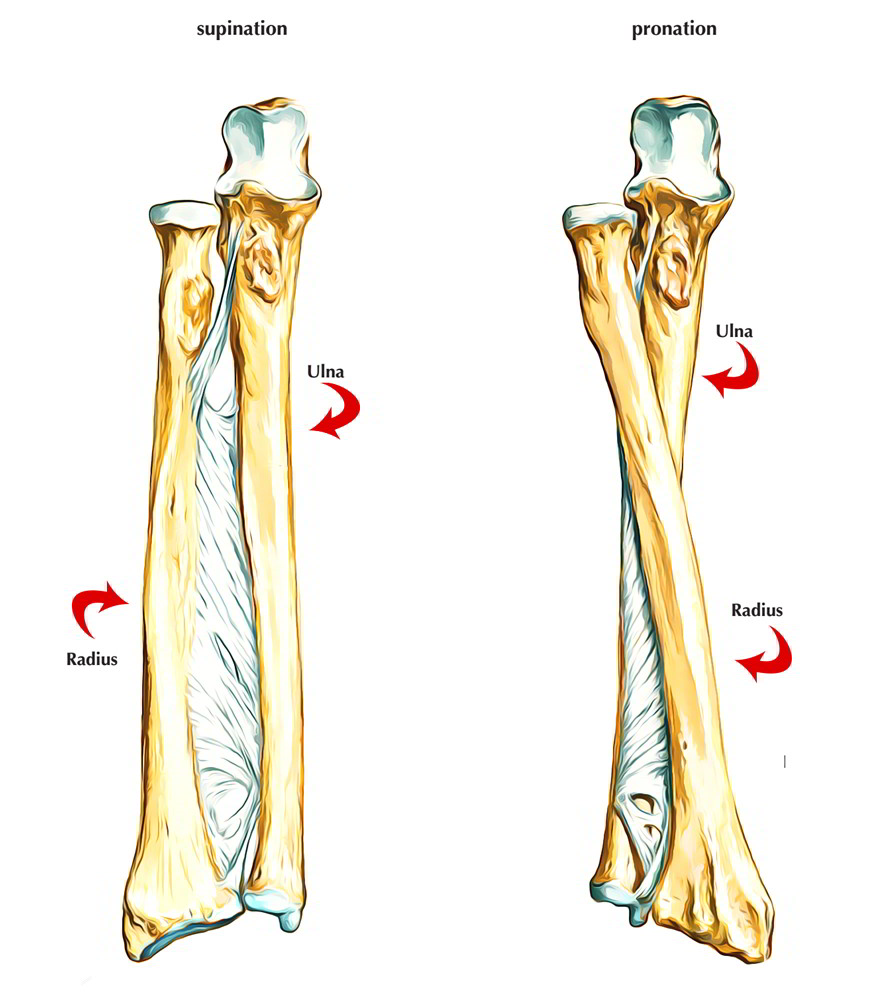
How Does The Radius Bone Move?
The radius is specially designed to rotate at the elbow and wrist joints along with, the ulna. During pronation, the distal end of the radius rotates around the ulna from its position on the lateral side of the wrist to the medial side of the wrist.
During supination, the supinator muscle of the forearm and the biceps brachii supinate the forearm by pulling the radius bone. This makes the radius move in the opposite direction of the pronator muscles, moving the distal end of the radius back to its position on the lateral side of the wrist.
Which Muscles Attaches To The Radius Bone?
In the image below pink color represents the origin and blue color represents the insertion of the muscles to the radius bone.
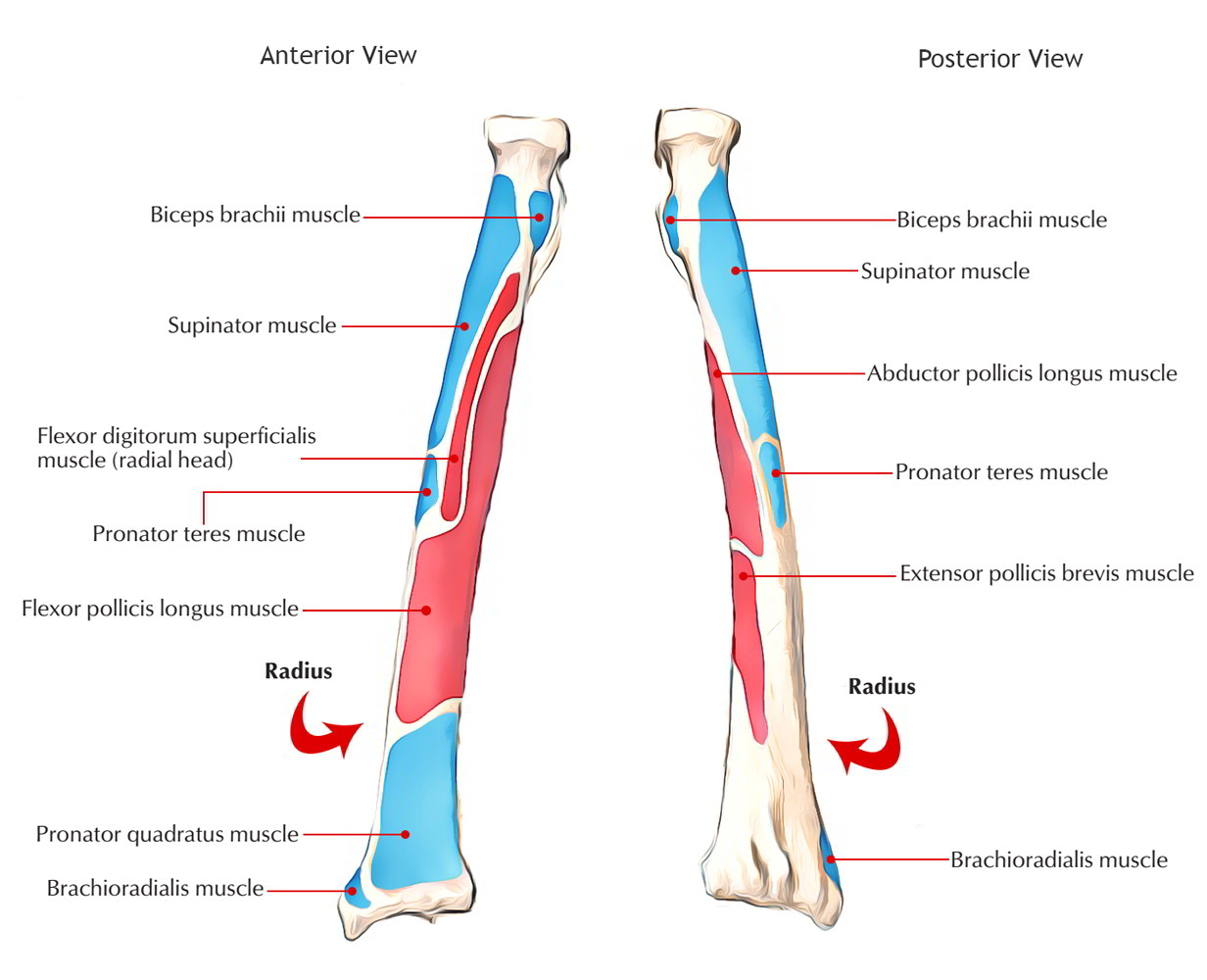
Muscles attached to radius bone
Muscles that originates from the radius bone are:
- Flexor pollicis longus muscle
- Flexor digitorum superficialis muscle (radial head)
- Abductor pollicis longus muscle
- Extensor pollicis brevis muscle
Muscles that inserts into the radius bone are:
- Biceps brachii
- Supinator muscle
- Pronator teres muscle
- Brachioradialis
- Pronator quadratus
From Where Does The Radius Bone Ossify?
The radius bone ossifies from three centers, one primary and two secondary.
The primary center of the radius bone shows up in the mid-shaft during 8th week of fetal life.
The secondary centers are for both upper end and lower end of the radius bone.
- The center for upper end of the radius bone shows up during fifth year.
- The center for lower end of the radius bone shows up at the age of first year.
The upper epiphysis merges at the age of 12 years. The lower epiphysis merges at the age of 20th year.
Sometimes an additional center is found in the radial tuberosity, which appears around 13th or 15th year.
What is The Clinical Significance of The Radius Bone?
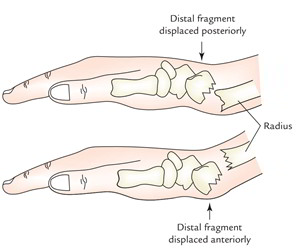
- In fracture shaft of radius bone, with fracture line below the insertion of biceps and above the insertion of pronator teres the upper fragment is supinated by supinator and lower fragment is pronated by the pronator teres.
- In fracture at the distal end of the radius bone (Colles’ fracture) the distal fragment is displaced backwards and upwards. The opposite of Colles’ fracture is referred to as Smith’s fracture.
- Fracture of styloid process of radius bone is termed ’Chauffeur’s fracture’.
Madelung deformity: It is a congenital defect of radius bone which provides the following clinical features: The anterior bowing of distal end of radius bone, as a result of an abnormal growth of distal epiphysis. It occurs between 10 and 14 years of age. There is premature disappearance of distal epiphyseal line. There may be subluxation or dislocation of distal end of ulna, because of defective development of distal radial epiphysis.
Ready For The Test?
Radius Bone


 (75 votes, average: 3.87 out of 5)
(75 votes, average: 3.87 out of 5)