The epidermis is a keratinized stratified squamous epithelium. An epithelium is avascular, meaning it lacks blood vessels. Since the epidermis is prone to injury, the lack of blood vessels prevents unnecessary found only in areas subjected to high levels of abrasion, such as the palms and soles.
The thickness of the epidermis ranges from 0.04 mm on the eyelids to 1.6 mm on the palms and soles. The keratinocytes within both thin and thick skin are so named because they undergo a process called keratinization, which leads to the eventual hardening and flattening of the cells through the production of keratin. Keratin is a tough, fibrous protein that provides waterproofing and abrasion protection for the skin.
The deepest layer of cells, the stratum basale, continuously produces new keratinocytes by mitotic cell division. As new cells are produced, the older cells superficial to them are gradually pushed toward the surface. The constant division of cells in the stratum basale enables the epidermis to repair itself when damaged. Upon leaving the stratum basale, keratinocytes enter the stratum spinosum. In this layer, keratinocytes begin to produce keratin within their cytoplasm. Neighboring cells also become physically connected, which creates a “spiny” appearance microscopically in fixed tissue.
As the keratinocytes continue to be pushed towards the epidermal surface, they leave the stratum spinosum and enter the stratum granulosum. The cells within this layer possess numerous granules that stain darkly in tissue section and are essential for the formation of keratin inside the cells. The cells within the stratum granulosum also undergo apoptosis, which is programmed cell death and involves the destruction of the nucleus and other organelles.
In thick skin, cells move superficially into the stratum lucidum. Because the cells in this layer do not have nuclei or organelles, this layer often appears “lucid” or transparent in section. The stratum lucidum is absent in thin skin, meaning cells move directly from the stratum granulosum into the most superficial layer of the epidermis, the stratum corneum (kor-ne-um). The stratum corneum is so named because it consists of approximately 20-40 layers of dead, squamous, and keratinized (cornified) cells. The superficial cells of the stratum corneum are continually being sloughed off and replaced by underlying cells moving towards the surface. The journey from stratum basale to stratum corneum usually takes seven to ten days, with cells remaining in the stratum corneum for another two weeks on average.
Skin coloration is due to both epidermal pigment accumulation and blood flow. The primary cutaneous pigment is melanin, synthesized in granules in epidermal melanocytes and a corresponding layer of the hair follicles. Skin color differences result from the size and quantity of granules as well as from the rate of melanin production. Natives of equatorial Africa have an increase in the size and number of granules as well as increased melanin production. In natives of northern Europe, the granules are small and aggregated, producing less melanin. With chronic sun exposure, there is an increase in the concentration of melanocytes as well as in size and functional activity. The presence of melanin limits the penetration of sun rays into the skin and protects against sunburn and development of ultraviolet light–induced skin carcinomas. Melanin that is produced in the epidermis can be deposited in the dermal skin layer through various processes (such as inflammation)
Three Types of Specialized Cells Are Also Present In The Epidermis.
Melanocytes are located in the stratum basale. They produce the brown-black pigment that is primarily responsible for skin color.
Dendritic (Langerhans)
cells are located in the strata spinosum and granulosum of the epidermis and are derived from monocytes, a type of white blood cell. These cells migrate throughout the epidermis where they use phagocytosis to remove pathogens trying to enter the body and alert the lymphoid system to launch an attack.
Tactile (Merkel)
cells in the stratum basale work with tactile discs in the dermis in touch sensation detection.
Blood flow to skin also imparts a tint reflecting the concentration and oxygenation of hemoglobin in the blood. Normally, oxygenated hemoglobin imparts a pinkish/reddish color. Severe restriction of cutaneous blood flow causes a whitish color, such as shock states. The presence of deoxygenated hemoglobin causes a bluish color. These colors may not be apparent in skin regions with high melanin content but can be seen in areas of relatively low melanin content such as the bed of the fingernail.
The epithelial barrier function is supplemented by hair and nails and secretions from sebaceous glands, eccrine glands, and apocrine sweat glands.These structures are invaginations of epidermis into the dermis.
Nails And Hair
Nails and hair consist of keratinized and, therefore, “dead” cells. Nails are horny scales of epidermis that grow from the nail matrix at the proximal nail bed. Fingernails grow about 1 mm/day, and complete reproduction takes 100 to 150 days. Toenails grow more slowly than do fingernails. A damaged nail matrix, which may result from trauma or aggressive manicuring, produces a distorted nail. Nails are also sensitive to physiologic changes; for instance, they grow more slowly in cold weather and during periods of illness.
Hair is found on all skin surfaces except the palms and soles. Each hair follicle functions as an independent unit and goes through intermittent stages of development and activity. Hair develops from the mitotic activity of the hair bulb. Hair form (straight or curly) depends on the shape of the hair in cross-section. Straight hair has a round cross-section; curly hair has an oval or ribbon-like cross-section. Curved follicles also affect the curliness of hair. Melanocytes in the bulb determine hair color.
Epidermal Glands
Three different types of glands are located in the epidermis. These glands are also composed of epithelial tissue; the glands themselves are secretory epithelia, and the ducts leading to the surface of the skin have exchange epithelia.
Sebaceous glands are found throughout the skin and are most abundant on the face, scalp, upper back, and chest. They are associated with hair follicles that open onto the skin surface, where sebum (a mixture of sebaceous gland- produced lipids and epidermal cell-derived lipids) is released. Sebum has a lubricating function and bactericidal activity. Androgen is responsible for sebaceous gland development. In utero androgen causes neonatal acne; after puberty, increased androgen production again stimulates sebum production, often leading to acne in adolescents.
Eccrine sweat glands play an important role in thermoregulation. They are found in most areas of the skin but are particularly numerous on the palms, soles, forehead, and axillae. Sweat is a dilute secretion derived from plasma. Eccrine gland secretion is stimulated by heat as well as by exercise and emotional stress.
Apocrine glands secrete cholesterol and triglycerides and occur primarily in the axillae, breast areola, anogenital area, ear canals, and eyelids. Sympathetic nerves stimulate apocrine secretion of a milky substance that becomes odoriferous when altered by skin surface bacteria. Apocrine glands do not function until puberty, and they require high levels of sex steroids in order to function. In lower order animals, apocrine secretions function as sexual attractants (pheromones), and the apocrine secretion musk is used as a perfume base. The role, if any, in humans is not established.
Accessory Structures
The accessory structures of the skin-hair, glands, and nails develop from the epidermis. These structures originate in either the dermis or the subcutaneous tissue because they develop from inward growths of the epidermis.
Summary of Accessory Structures
| Structure | Origin | Function |
| Hair | Fused keratinized epidermal cells formed at base of hair follicle | Scalp hair: protects scalp from excessive heat loss, mechanical injury, and UV radiation Eyelashes and eyebrows: protect eyes from sunlight and dust |
| Ear and nasal hairs: keep dust and insects out of the external acoustic meatus and nasal cavity | ||
| Sebaceous glands | Formed as an epidermal out pocketing from a hair follicle | Produce sebum to prevent excessive dryness of hair and skin, inhibit microbial growth on skin surface, and reduce evaporative water loss |
| Sweat glands | Apocrine sweat glands formed as an epidermal outpocketing from hair follicles in axillary, areolar, beard, and genital regions | Produce a sweat that contains human pheromones |
| Eccrine sweat glands formed as epidermal ingrowth | Produce sweat that cools the body through evaporation, protects from pathogens through lysozyme, has an acidic pH, provides a flushing action, and makes minor contribution to waste removal | |
| Ceruminous glands | Modified sweat glands | Produce waxy cerumen to keep eardrum moist and capture particles and insects entering external acoustic meatus |
| Nails | Fused keratinized epidermal cells formed within an ingrowth of the epidermis | Protect the distal surfaces of fingers and toes; manipulating small objects |
Hair
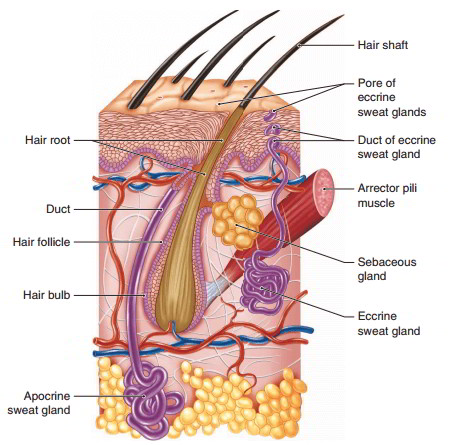
A hair is formed of keratinized cells and consists of two parts: a shaft and a root. The hair shaft is the portion that projects above the skin surface. The hair root lies below the skin surface in a hair follicle, an inward, tubular extension of the epidermis. The follicle penetrates into the dermis and usually into the subcutaneous tissue. The region of cell division, where the stratum basale forms new hair cells, is located in the hair bulb (base) of the follicle. The hair bulb is enlarged where it fits over a dermal papilla, which contains blood vessels that nourish the dividing epidermal cells. The hair cells become keratinized, die, and become part of the hair root. The continuing production of new cells causes growth of the hair.
Each hair follicle has an associated arrector pili muscle that is attached at one end to the deeper portion of a hair follicle and to the papillary layer of the dermis at the other end . Each muscle is a small group of smooth muscle cells. When a person is frightened or very cold, the arrector pili muscles contract and raise the hairs on end, producing goose bumps or chicken skin. Though of little value in humans, the erect hairs express rage to enemies or increase the thickness of the insulating layer of hair in cold weather in many mammals.
Hair is present over most of the body, but it is absent on the soles, palms, nipples, lips, and portions of the external genitalia. Its primary function is protection, although the tiny hairs over much of the body have little function. Eyelashes and eyebrows shield the eyes from sunlight and foreign particles. Hair in the nostrils and external acoustic meatuses (ear canals) act as filters to protect against the entrance of foreign particles and insects. Hair protects the scalp from sunlight, mechanical injury, and heat loss. The hair root plexus wrapping around the hair follicle detects
movement of the hair shaft when skin contact is made.
Normal hair loss from the scalp is about 75 to 100 hairs per day. Hair loss is increased and regeneration is decreased by poor diet, major illnesses, emotional stress, high fever, certain drugs, chemical therapy, radiation therapy, and aging. Baldness, an inherited trait, is much more common in males than in females.
Glands
Exocrine glands associated with the skin are of three types: sebaceous (oil), sweat, and cerumi nous (wax) glands. Each type of gland is formed by an inward growth of the epidermis during embryonic development.
Sebaceous Glands
Sebaceous (se-ba-shus) glands are oil-producing glands that usually empty their oily secretions into hair follicles. The oily secretion, called sebum, moves superficially along the hair root until it reaches the skin surface. Sebum helps to protect the body by inhibiting the growth of some pathogens on the skin surface and by keeping the hair and skin pliable and soft. Moisturizing the skin keeps it from becoming dry and cracked, which creates passageways for pathogens to enter the body. It also aids in preventing dehydration by reducing evaporative water loss. Sebaceous glands increase their production of sebum at puberty. Accumulated sebum in enlarged hair follicles may form blackheads, whose color comes from oxidized sebum and melanin and not from dirt as is commonly believed. Invasion of certain bacteria may result in pimples or boils.
Sweat Glands
Sweat glands play an important role in maintaining homeostasis. The two types of sweat glands are apocrine sweat glands and eccrine (or merocrine) sweat glands. Both types of glands are tubular in shape, similar to a garden hose. The secretory portion of both types of sweat glands is coiled and located within the dermis and subcutaneous tissue, with the apocrine type located deeper than the eccrine type. In addition to being richly supplied with blood vessels, each sweat gland possesses a relatively straight, narrow duct that carries the glandular secretion to either the skin surface or a hair follicle.
Eccrine (ek’-rin) sweat glands are the most abundant skin glands, with over two million scattered across the body surface. The clear, watery sweat produced is delivered through a narrow duct directly to the skin surface. Eccrine sweat glands are active from birth and are stimulated to produce sweat when body temperature starts to rise during activities such as exercise. The watery nature of eccrine sweat assists in cooling the body through evaporation from the skin surface. Eccrine sweat is capable of protecting the body from environmental hazards. It contains a chemical called lysozyme, which has the ability to kill certain types of bacteria on the skin surface. The slightly acidic nature of eccrine sweat limits pathogen growth on the skin surface. Also the large volume of sweat that can be produced creates a flushing action that can wash chemicals, pathogens, dirt, etc. from the skin surface. Although the kidneys and lungs are the primary organs of excretion, eccrine sweat does contain small amounts of salts and wastes, in addition to other substances that happen to be in excess within the blood. For example, glucose (blood sugar) can be detected in the sweat of individuals with diabetes mellitus.
Apocrine (ap ‘-o-krin) sweat glands have ducts that empty secretions into hair follicles. They occur primarily in the axillary, areolar, beard, and genital regions and become active at puberty under the influence of the sex hormones. These glands become activated during times of emotional stress and sexual excitement. Apocrine sweat is viscous and milky in color, due to the addition of lipid and proteins. Although the secretions are essentially odorless, decomposition by bacteria produces waste products that cause body odor. Apocrine sweat also contains pheromones, chemicals with the ability to alter physiological processes in nearby organisms. Studies have demonstrated the ability of human pheromones to affect reproductive function in males and females.
Ceruminous Glands
Ceruminous (se-ru’mi-nus) glands are modified apocrine sweat glands that are located in the external acoustic meatus and produce a waxy secretion called cerumen. The sticky, waxy nature of cerumen helps to keep foreign particles and insects out of the external acoustic meatus. Occasionally, excessive production of cerumen causes a buildup of wax that becomes impacted in the external acoustic meatus. This condition may cause a slight hearing loss as well as pain. Once the impacted wax is removed by irrigation and/or mechanical means, hearing returns to normal.
Nails
Hard, hooflike nails, composed of dead keratinized epidermal cells, cover the distal surfaces of the fingers and toes. A nail consists of a nail body, the portion that is visible, and a nail root, the proximal portion that is inserted into the dermis. Nails are colorless but they normally appear pinkish due to the blood vessels in the nail bed, which is the skin deep to the nail body. Nails appear bluish in persons suffering from severe anemia or oxygen deficiency. Near the nail, root is a whitish, crescent-shaped area that is called the lunula. The cuticle is a band of epidermis attached to the proximal border of the nail body. The major function of nails is protection, but fingernails are also useful in manipulating small objects.