The Anal Canal is the terminal part (3.8 cm long) of the large intestine, situated in the perineum below the pelvic diaphragm. Like rectum it’s devoid of sacculations, taenia coli, and appendices epiploicae. It’s encompassed by an inner automatic sphincter and an outer voluntary sphincter, whose tone keeps the anal canal closed with the exception of during the defecation.
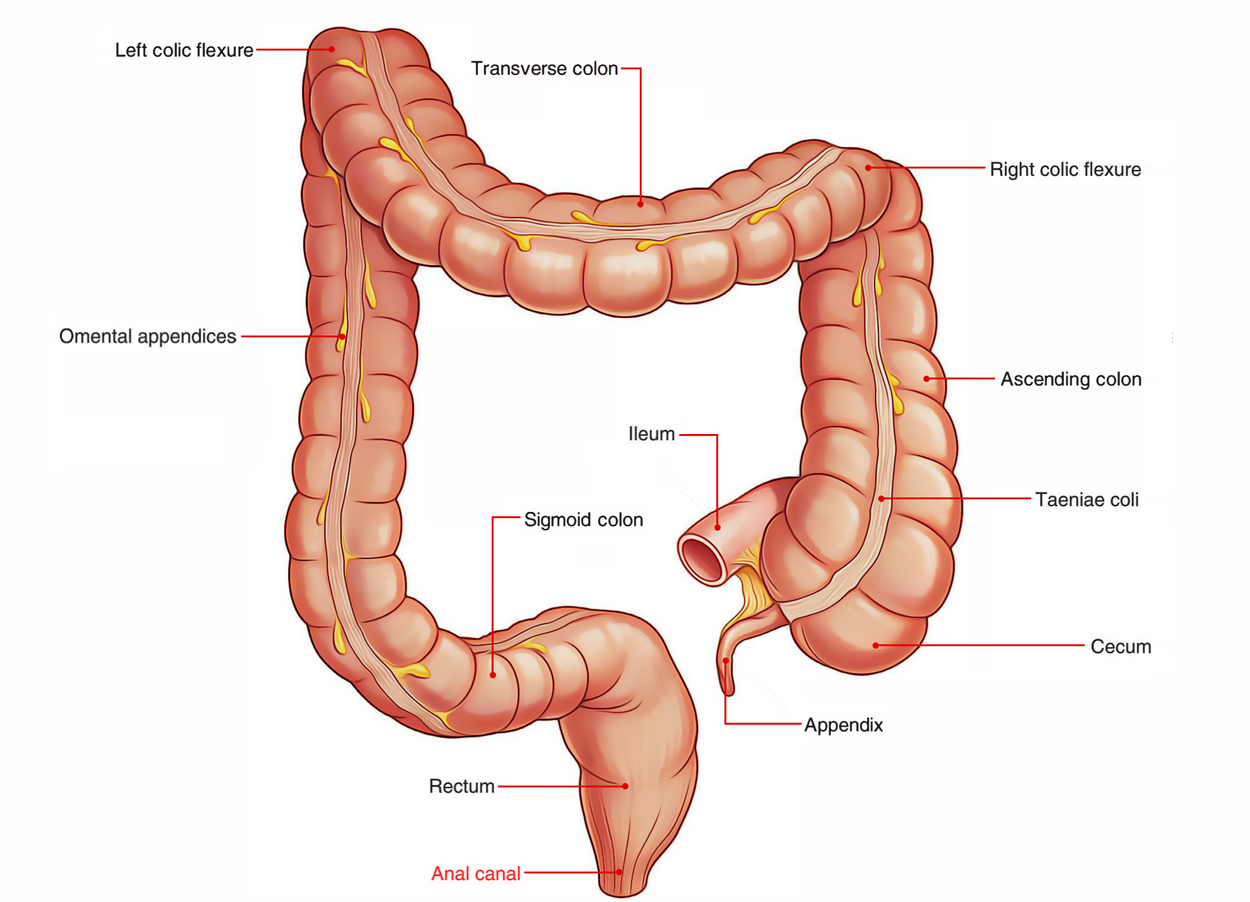
Anal Canal
Location
The anal canal is situated in the anal triangle of the perineum between the left and right fat filled up ischiorectal fossae. These fossae enable the growth of the anal canal during defecation.
Extent and Course
The anal canal commences at the anorectal junction, enters downward and backward, and opens at the anal orifice, that is situated in the natal cleft (cleft between the buttocks) about 4 cm below and in front of the tip of coccyx. The skin enclosing the anal orifice is pigmented and thrown into radiating folds because of pull used by underlying subcutaneous muscle- the corrugator cutis ani.
The anorectal junction is encompassed by puborectalis which pulls it forwards creating, forwards convexity and backward fold of 90 ° (perineal flexure).
Interior of the Anal Canalprovid
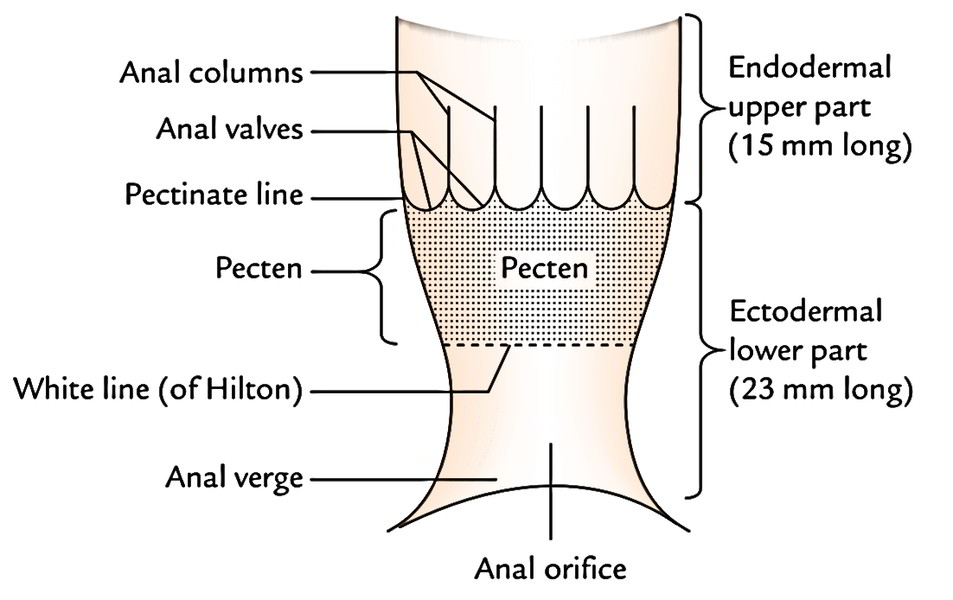
Anal Canal: Interior
The anal canal is split into upper and lower parts by the pectinate line. The pectinate line represents the embryological site of connection of the anal membrane.
The upper part of the anal canal stretches from the anorectal junction to the pectinate line; and the lower part of the anal canal stretches from the pectinate line to the anal verge.
The upper and lower parts of the anal canal are distinct in development, blood supply, lymphatic drainage, and Nerve Supply.
Differences between the Upper and Lower Anal Canals
| Features | Upper anal canal | Lower anal canal |
|---|---|---|
| Development | From endoderm of the hind gut | From ectoderm of proctodeum |
| Innervation | Autonomic nerves, hence insensitive to pain and temperature | Somatic nerves, hence sensitive to pain and temperature |
| Epithelial lining | Simple columnar | Stratified squamous |
| Arterial supply | Superior rectal artery | Inferior rectal artery |
| Venous drainage | Superior rectal vein draining into portal system | Inferior rectal vein draining into caval system |
| Lymphatic drainage | Internal iliac lymph nodes | Superficial inguinal lymph nodes (horizontal set) |
| Hemorrhoids | Internal hemorrhoids | External hemorrhoids |
Features in the Upper Part of Anal Canal
The upper part of the anal canal (15 millimeters long) presents these features:
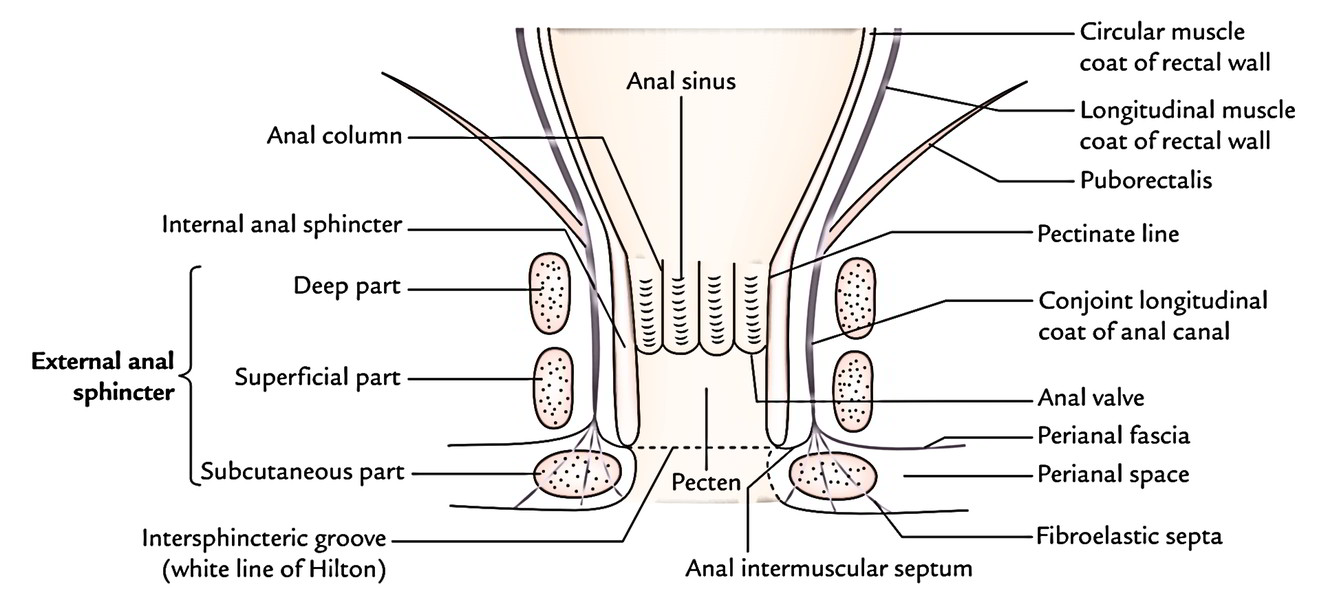
- Anal Pillars (Pillars of Morgagni): All these are long-lasting longitudinal mucous folds numbering 6 to 10. They include radicles of the superior rectal vein.
- Anal valves (valves of Morgagni): All these are crescentic folds of the mucous membrane which attach the lower ends of adjacent anal Pillars. The complimentary margins of these valves are directed upward. The position of these valves is suggested by the wavy pectinate line (also referred to as dentate line).
- Anal sinuses: All these are vertical recesses between the anal Pillars and above the anal valves. The ducts of tubular anal glands existing in the submucosa open in the floor of anal sinuses.
Relationships
All these are as follows:
Anteriorly:
- Perineal body.
- Bulb of penis and spongy urethra in male and lower part of the vagina in female.
Posteriorly:
- Anococcygeal raphe.
- Tip of coccyx.
- Fibrofatty tissue between the perineal skin and the anococcygeal raphe.
Laterally (on every side):
- Ischiorectal fossa.
Features in the Lower part of Anal Canal
The lower anal canal is further split into 2 regions: upper and lower.
- Upper region (frequently named pecten): It’s 15 millimeters long and stretches from the pectinate line to Hilton’s line. It’s lined by the non-keratinized stratified squamous epithelium. The mucous lining in this region appears bluish in colour because of underlying dense venous plexus and is adherent to the underlying structures.
- Lower region of lower anal canal: It’s about 8 mm in extent and lined by the true skin consisting of sweat and sebaceous gland. It reveals pigmentation. In adult males, rough hairs are frequently seen around the anal orifice.
Hiltons line: The white line of Hilton is situated in the junction of the subcutaneous external anal sphincter and the lower end of internal anal sphincter, and represented by the anal intersphincteric groove. It presents these features:
- It demarcates mucocutaneous junction.
- It seems white since it is located between the bluish pinkish area above and blackish skin below, for this reason the name white line of Hilton.
Anal Sphincters
There are just two sphincters, (internal and external), around the anal canal, which supply strong sphincteric mechanism in the distal end of the gastrointestinal tract.
Internal Sphincter
- It’s created by thickened circular muscle layer of the anal canal and encompasses the upper two-third of the canal.
- Above, it’s constant with the circular muscle layer of the rectum and below reaches up to the level of the white line of Hilton.
- It’s encircled by the deep and superficial parts of the external anal sphincter.
External Sphincter
The external anal sphincter as the particular name indicates is outside the internal anal sphincter. It encircles the entire length of the anal canal and is composed of 3 parts: deep, superficial, and subcutaneous.
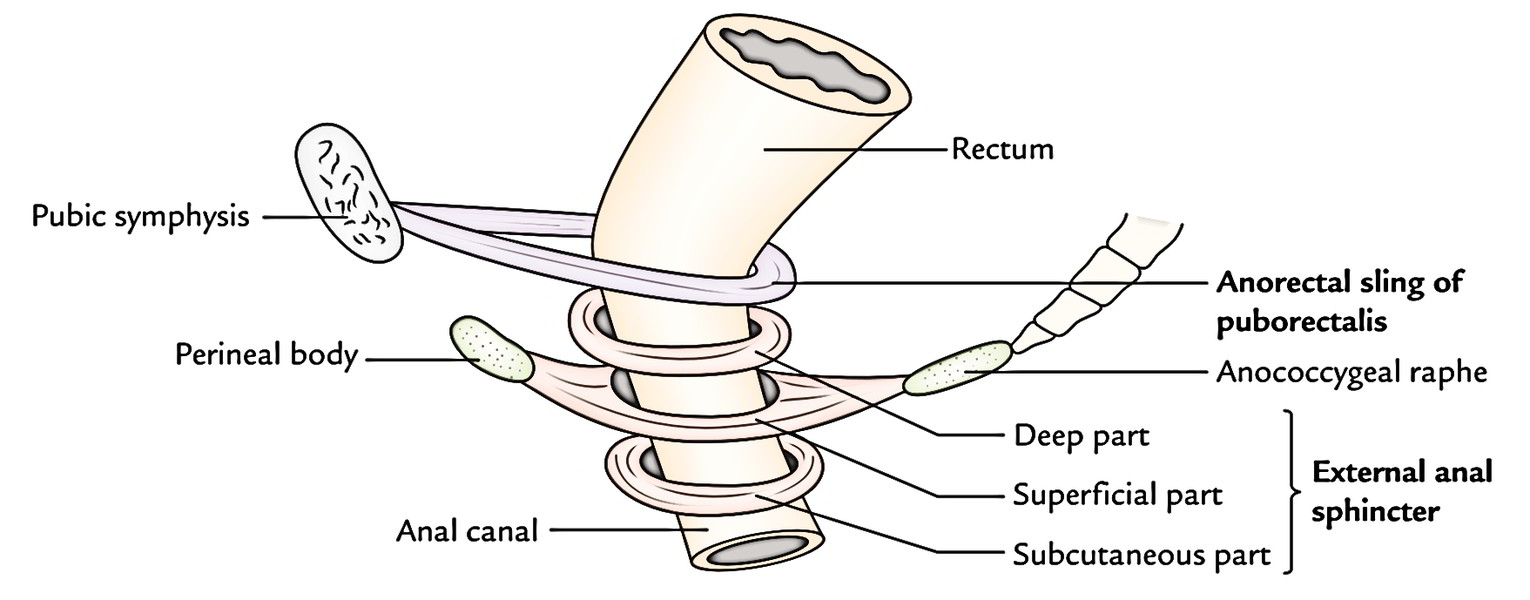
Anal Canal: External Sphincter
Deep Part
The deep part encompasses the upper part of the internal sphincter. It’s no bony attachments. The puborectalis mixes with the deep part of external sphincter behind and creates a sling around the anorectal junction, which is connected anteriorly to the rear of the pubis. In the resting state, the anorectal tube is angled forwards at this level and contraction of puborectalis sling will raise this angle, a significant determinant in the continence mechanism.
Superficial Part
The superficial part is elliptical in shape. It originates from the tip of coccyx and anococcygeal raphe behind, encompasses the lower part of internal sphincter and after that gets added into the perineal body in front.
Subcutaneous Part
The subcutaneous part is located below the internal sphincter in the perianal space and encompasses the lower part of the anal canal. It’s the creation of flat band, about 15 mm broad. It’s no bony connection. It’s traversed by fibroblastic septa originated from the conjoint longitudinal jacket.
Nerve Supply of the Sphincter
- The internal sphincter is composed of smooth muscle and furnished by the autonomic nerve fibres (sympathetic and parasympathetic), thus it’s involuntary.
- The external anal sphincter is composed of striated muscle and thus, supplied by the somatic nerve- inferior rectal nerve and perineal branch of 4th sacral nerve. It’s consequently under voluntary control.
Anorectal ring: While doing per rectal examination, the muscular ring on which the bent finger rests just over an inch above the anal margin is the “anorectal ring”. It’s created by the fusion of the deep part of the external sphincter, the internal sphincter, and puborectalis, and demarcates the junction between the anal canal and the rectum. Surgical excision of the ring leads to incontinence.
Conjoint longitudinal jacket of the anal canal: It’s created at the anorectal junction by the fusion of puborectalis and longitudinal muscle layer of the rectal wall. It runs vertically downward between the internal and external anal sphincters, and in the level of white line it breaks up into a number of fibroelastic septa which fan out, traverse via the subcutaneous part of the anal canal to be connected to the skin around the anal orifice. The most lateral of these septa creates perianal fascia which enters laterally to be connected to obturator fascia enclosing the pudendal canal. The space between the perianal fascia and the skin is named perineal space. The most medial septum of the conjoint longitudinal coating creates the anal intermuscular septum, which enters medially and gets connected to Hilton’s line.
Surgical Spaces related to the Anal Canal
All these are 2 ischiorectal fossae, perianal space, and submucous space of the anal canal.
- Ischiorectal spaces or fossae: They are located 1 on every side of the anal canal and are filled up with fat.
- Perianal space: It encompasses the anal canal below Hilton’s line. It is located between the perianal fascia and skin. It includes the subcutaneous part of anal sphincter, lobulated fat, external rectal venous plexus, and terminal branches of the inferior rectal nerve and vessels. The perianal abscess is quite distressing.
- Submucous space of anal canal: It is located above the white line of Hilton between the mucous membrane and the internal anal sphincter, and includes internal rectal venous plexus.
Arterial Supply
The upper part of anal canal is supplied by the superior rectal artery and the lower part of anal canal is supplied by the inferior rectal artery.
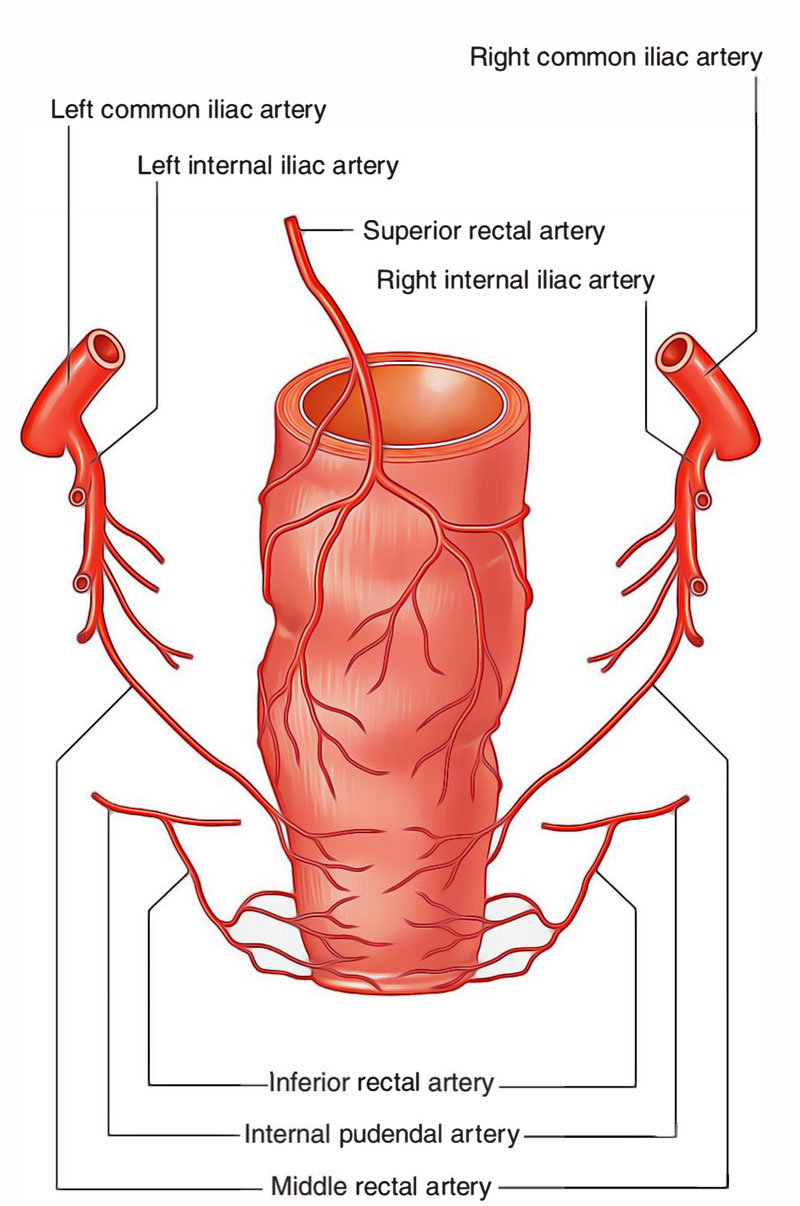
Anal Canal: Arterial Supply
Venous Drainage
The upper part of the anal canal is emptied into the portal venous system by the superior rectal vein and the lower part of the anal canal is emptied into the caval (systemic) system by inferior rectal veins.
Lymphatic Drainage
The upper part of the anal canal empties into the internal iliac nodes on the other hand the lower part drains into the horizontal group of superficial inguinal nodes. Thus, the pectinate line creates the “water shed line” of the anal canal.
Development
The upper part of the anal canal is endodermal in origin and grows from anorectal canal (dorsal part of cloaca) and lower part of the anal canal is ectodermal in origin and develops from proctodeum. The anal membrane dividing both parts breaks down at birth. Its remains are represented by the pectinate line in the anal canal. The anal valves are reported to be the remains of the anal membrane.
Clinical Significance
Hemorrhoids (or Piles)
All these are variceal dilatations of the submucosal anal and perianal venous plexuses. They’re classified into 2 types:
Internal Hemorrhoids (or True Hemorrhoid).
- All these really are the saccular dilatations of the tributaries of the superior rectal (hemorrhoidal) vein above the pectinate line in portal vein obstacle. The internal hemorrhoids could be primary or secondary. The primary piles are created because of dilatations of principal tributaries/radicles of the superior rectal vein which is located in the anal Pillars which inhabit the left lateral, right posterior, and right anterior postures.
- The dilatations of radicles of superior rectal vein in other postures are referred to as secondary hemorrhoid. The location of primary hemorrhoid corresponds to the 3 o’clock, 7 o’clock, and 11 o’clock Positions of the anal wall, when seeing the inside of anal canal in lithotomy position.
- Anatomically every hemorrhoids/ heap is composed of fold of mucosa and submucosa consisting of a varicose radicle of the superior rectal vein and a terminal branch of the superior rectal artery.
- They’re painless but bleed profusely on straining during defecation (passing fecal matter).
- Types: Initially they’re confined inside the anal canal (1st level), slowly they enlarge and prolapse during defecation (2nd level), and ultimately stay prolapsed (3rd degree).
External Hemorrhoids (or Fake Hemorrhoid).
- These are dilatations of the tributaries of inferior rectal vein below the pectinate line. They’re covered by the mucous membrane of the lower half of the canal. They’re quite debilitating and don’t bleed on straining during defecation.
- The so-called thrombosed external heap is a small stressed hematoma in the anal margin caused because of rupture of the subcutaneous vein. For this reason, it ought to be truly called perianal hematoma.
Fissure in Anorectal Canal
It’s caused by rupture of 1 of the anal valves (valves of Morgagni) by the passage of tough fecal mass. They take place posteriorly in the midline and are quite distressing since the inferior aspect of the valve is lined by the mucous membrane/skin of the lower half of anal canal supplied by the somatic nerves.
Fistula in Anorectal Canal
It’s caused by the rupture of an abscess around the canal. The abscess opens spontaneously internally into the anal canal and externally on the surface and the track becomes epithelialized. Low level anal fistula going through the lower part of the superficial anal sphincter is the most frequent.

 (55 votes, average: 4.56 out of 5)
(55 votes, average: 4.56 out of 5)