Scrotum is a large pendulous sac of skin below and behind the penis. Scrotum is known as ‘bag’ in latin. It is also referred as an out-pouching of the lower part of the anterior abdominal wall. It is comprised of the following structures:
- Testes.
- Epididymis.
- Lower parts of the spermatic cords.
External Features
The scrotum presents the following external features:
- The scrotum is split into left and right halves by a median ridge or raphe, which suggests the line of fusion of the 2 halves of the scrotum. This ridge is continued forwards in the midline to the undersurface of the penis and backwards in the midline of the perineum to the anus.
- The skin is rugose (corrugated) and dark in colour. The rugosity of the skin takes place because of the presence of subcutaneous dartos muscle.
- The left half of the scrotum hangs lower compared to the right half, as the left spermatic cord is longer in relation to the right spermatic cord.
Layers of The Scrotum
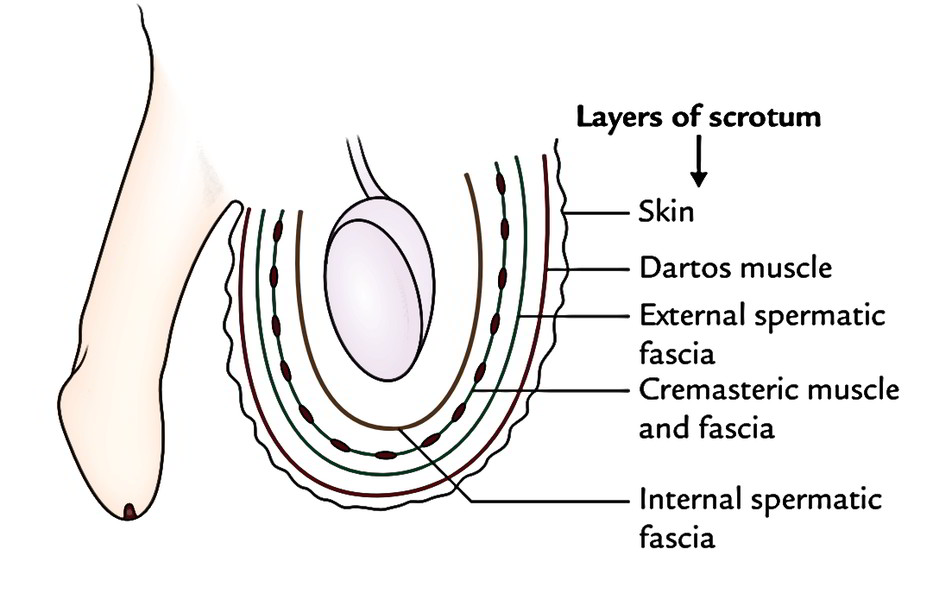
The scrotal wall from without inward is created from the following 5 layers:
- Skin.
- Dartos muscle (which replaces the superficial fascia).
- External spermatic fascia.
- Cremasteric muscle and fascia.
- Internal spermatic fascia.
The cavity of the scrotum is partially split into 2 halves, left and right, by a septum; the dartos muscle extends into this septum. Every half of the scrotal cavity includes the testis, epididymis, and lower part of the spermatic cord of the corresponding side.
The scrotal skin
It is thin, elastic, pigmented and presence of rugose due to adhesion with the
underlying dartos muscle. It bears scatted coarse hairs and numerous sebaceous and sweat glands, pigment cells, nerve endings. Here the absence of subcutaneous adipose tissue helps in lowering the scrotal temperature.
Dartos muscle
- It is the thin layer of subcutaneous involuntary muscle
- It is continuous with the fascia of camper and scarpa of the anterior abdominal wall and posteriorly with the fascia of colles of the perineum
- It extends interiorly at the median raphe as scrotal septum
- Tis layer helps in regulation of temperature within the scrotum.
External spermatic fascia
- It is the tubular prolongation of the fibrous tissue from the margins of the superficial inguinal ring
- It is the continuation of apponeurosis of external obliquus abdominis and overlying fascia.
Cremasteric muscle and fascia
- It is derived from the obliquus abdominis and transversus abdomonis
- It extends from the superficial inguinal ring, and spreads in the scrotum in form of U-shaped loops which are held together by an areolar fascia
- When this muscle contracts, it pulls the testis towards superficial inguinal ring and acting as cremasteric plug.
Internal spermatic fascia
It is derived from the fascia transversalis from the margins of the deep inguinal ring.
The parietal layer of tunica vaginalis
It is developed from the distal part of the processus vaginalis of the peritoneum.
Comparison Between The Layers of The Anterior Abdominal Wall And The Scrotum
Layer of anterior abdominal wall | Layer of scrotum |
|---|---|
| Skin | Skin |
| Superficial fascia | Dartos muscle |
| External oblique muscle | External spermatic fascia |
| Internal oblique muscle | Cremasteric muscle and fascia |
The subcutaneous dartos muscle helps in the regulation of temperature inside the scrotal cavity. Remember the testis wants suitable temperature for properspermatogenesis. For this reason, during the summertime below the sway of heat, the relaxed scrotum becomes flaccid and elongated. Contrary to this, in the winter season below the sway of cold, dartos muscle contracts and scrotum becomes rounded and small with increased skin rugosity.
Blood Supply
The following arteries provide the scrotum:
- Superficial external pudendal artery.
- Deep external pudendal artery.
- Scrotal branches of the internal pudendal artery.
- Cremasteric artery, a branch of the inferior epigastric artery.
Nerve Supply
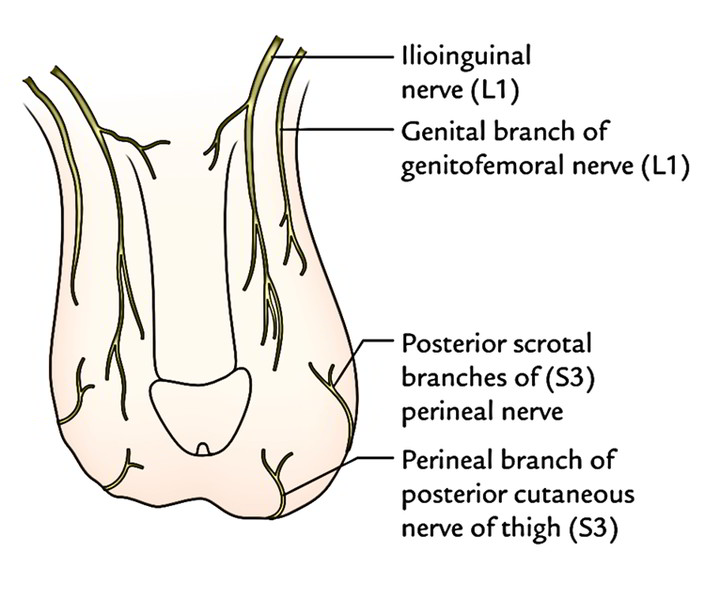
- Anterior 1-third of the scrotum is provided by ilioinguinal nerve (L1) and genital branch of genitofemoral nerve (L1).
- Posterior 2-third of the scrotum is provided by posterior scrotal branches of the perineal nerve (S3) and perineal branch of the posterior cutaneous nerve of the thigh (S3).
- The automatic dartos muscle is provided by the sympathetic fibres via genital branch of the genitofemoral nerve.
- The regions provided by L1 and S3 spinal sections are split by the ventral axial line.
Lymphatic Drainage
The lymph vessels from the scrotum drain into the superficial inguinal lymph nodes.
Development
The scrotum grows from labioscrotal swellings and urogenital folds, which fuse in the midline to create the scrotum. The site of fusion of urogenital folds is indicated by midline fibrous ridge/raphe on the scrotum. The labioscrotal folds in the female create the labia majora and urogenital folds stay different and create the labia minora.
Clinical Significance
Scrotal Edema
The scrotum is a familiar site of edema as a result of laxity of the skin and its dependent position.
Sebaceous Cysts
These frequently happen in the scrotum as a result of presence of a large number of hair and sebaceous glands in the scrotum.
Scrotal Elephantiasis
It’s a clinical condition characterized by a huge swelling and enlargement of the scrotum because of accumulation of interstitial fluid in the scrotal wall following blockage of lymph vessels by slim worms of filariasis (Wuchereria bancrofti).

 (50 votes, average: 4.72 out of 5)
(50 votes, average: 4.72 out of 5)