Esophagus is a narrow muscular tube extending from pharynx to the stomach. It gives passage for chewed food (bolus) and liquids during the third stage of deglutition and is about 25 cm long. Its engagement in different diseases like esophagitis, esophageal varices and cancer makes the anatomy of esophagus medically significant. It begins with lower part of the neck and ends in the upper part of the abdomen by joining the upper end of the stomach.
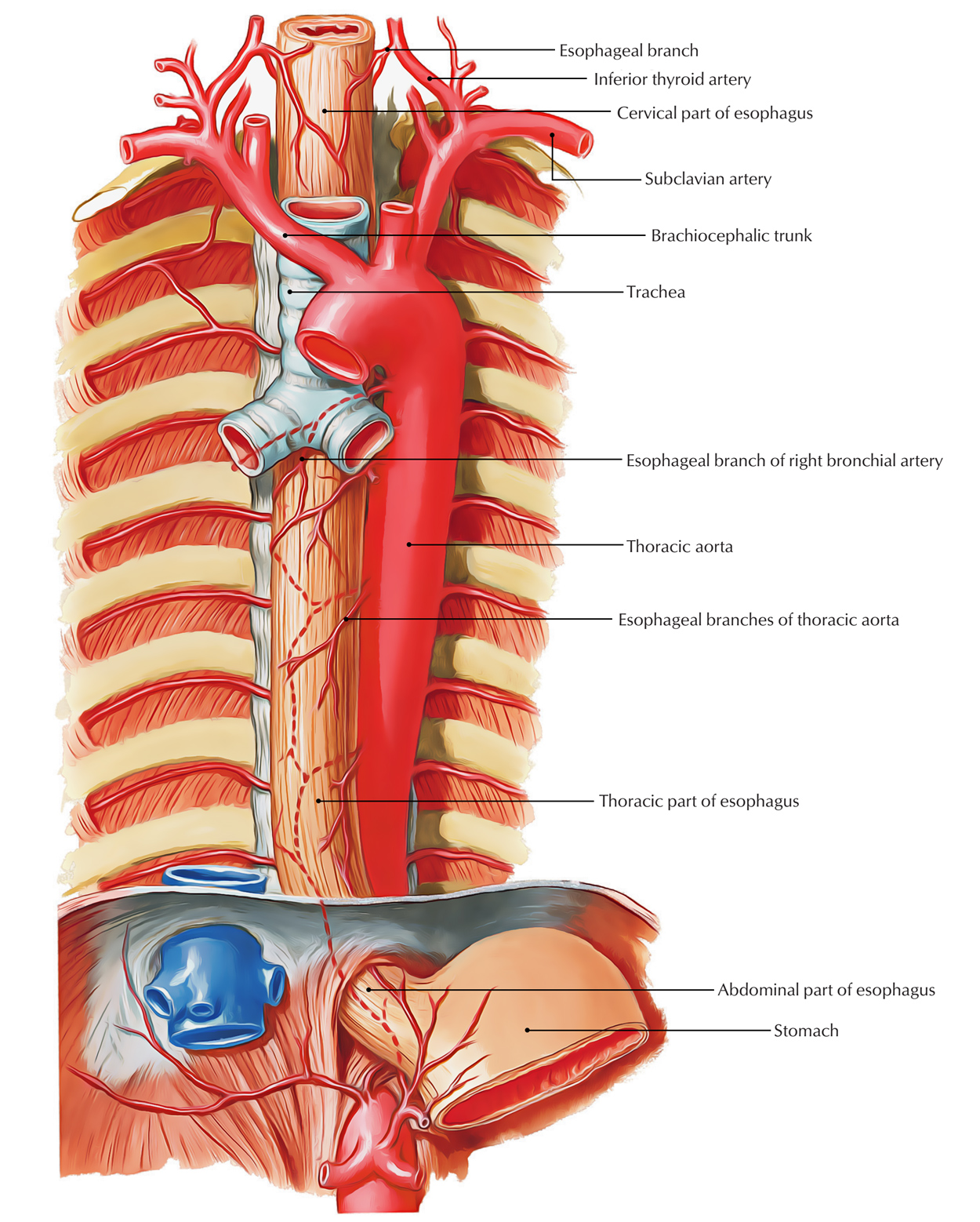
Esophagus
Dimensions and Lumen
Length: 25 cm (10 inches).
Width: 2 cm.
Lumen: It’s flattened anteroposteriorly. Normally it’s kept closed (collapsed) and opens (dilates) only during the passage of the food.
Course
The esophagus begins in the neck at the lower border of the cricoid cartilage (at the lower border of C6 vertebra), descends in front of the vertebral column goes through superior and posterior mediastina, pierces diaphragm in the level of T10 vertebra and ends in the abdomen in the cardiac orifice of the stomach in the level of T11 vertebra.
Curvatures
The cervical portion of esophagus commences in the mid line, then inclines somewhat to the left of the mid line in the root of neck, enters the thoracic inlet, enters through superior mediastinum. At the level of T5 vertebra, it returns to the mid line, but at T7 it again deviates to the left and inclines forwards to pass in front of the descending thoracic aorta and pierces diaphragm 2.5 cm to the left of the mid line (a thumbs breadth from the side of sternum), at the level of 7th left costal cartilage. Here fibres of the right crus of diaphragm sweep around the esophageal opening creating a sling around the esophagus. It enters the abdomen to join the stomach in the level of T11 vertebra. Thus esophagus presents the following curvatures:
A. Two side-to-side curvatures, both in the direction of the left:
- First at the root of the neck, before entering the thoracic inlet.
- Second at the level of T7 vertebra, before passing in front of the descending thoracic aorta.
B. Two anteroposterior curvature:
- First corresponding to the curvature of cervical spine.
- Second corresponding to the curvature of thoracic spine.
Constrictions
Normally, there are 4 sites of anatomical constrictions/ narrow parts in the esophagus. The distance of each constriction is measured from the upper incisor teeth. The constrictions are as follows:
- First constriction, at the pharyngo-esophageal junction, 9 cm (6 inches) from the incisor teeth.
- Second constriction, where it’s crossed by the arch of aorta, 22.5 cm (9 inches) from the incisor teeth.
- Third constriction, where it’s crossed by the left principal bronchus, 27.5 cm (11 inches) from the incisor teeth.
- Fourth constriction, where it pierces the diaphragm, 40 cm (15 inches) from the incisor teeth.
The sites of constriction, their respective distances from the upper incisor teeth and their vertebral level are given below:
Sites Of Constriction In The Esophagus
Site of constriction
Vertebral level Distance from upper incisor teeth At the pharyngo-esophageal junction (cervical constriction) C6 6 inches (15 cm) At crossing of arch of aorta (aortic constriction) T4 9 inches (22 cm) At crossing of left principal bronchus (bronchial constriction) T6 11 inches (27 cm) At the opening in the diaphragm (diaphragmatic constriction) T10 15 inches (40 cm)
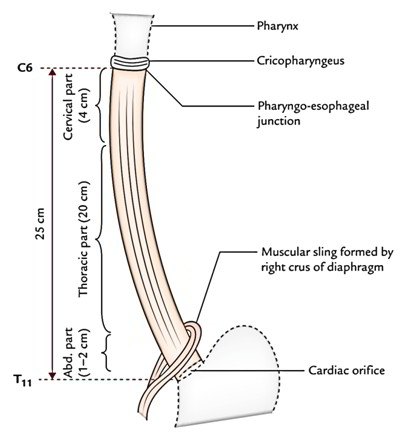
Parts Of The Esophagus
The esophagus is split into the following 3 parts:
- Cervical part (4 cm in length).
- Thoracic part (20 cm in length).
- Abdominal part (12 cm in length).
The cervical part extends from the lower border of cricoid cartilage to the superior border of manubrium sterni.
The thoracic part extends from superior border of manubrium sterni to the esophageal opening in the diaphragm.
The narrowest part of esophagus is its commencement at the cricopharyngeal sphincter.
The abdominal part extends create esophageal opening in the diaphragm to the cardiac end of the stomach.
Relations
Relationships of the Cervical Part of the Esophagus
Anteriorly, it’s related to:
- Trachea and
- recurrent laryngeal nerve
Posteriorly, it’s related to:
- prevertebral fascia
- longus colli muscles
- vertebral column
The prevertebral layer of deep cervical fascia creates a movable base on which the trachea and esophagus move up and down during swallowing and phonation.
On every side, it’s related to:
- lobe of the thyroid gland
- common carotid artery and
- thoracic duct on the left side
Relations Of Thoracic Part Of The Esophagus
Anterior: From above downwards these are as follows:
- Trachea.
- Arch of aorta.
- Right pulmonary artery.
- Left principal bronchus.
- Left atrium enclosed in the pericardium.
- Diaphragm.
Posterior:
- Vertebral column.
- Right posterior intercostal arteries.
- Thoracic duct.
- Azygos vein.
- Hemiazygos veins (terminal parts).
- Descending thoracic aorta.
To the right:
- Right lung and pleura.
- Azygos vein.
- Right vagus nerve.
To the left:
- Arch of aorta.
- Left subclavian artery.
- Thoracic duct.
- Left lung and pleura.
- Left recurrent laryngeal nerve.
- Descending thoracic aorta.
Relations Of Abdominal Part Of The Esophagus
Anterior:
- Posterior surface of the left lobe of the liver.
- Left gastric nerve.
Posterior:
- Left crus of diaphragm.
- Right gastric nerve.
The abdominal part of esophagus is shortest (1 to 2 cm long) and is the only part covered with serous membrane – the peritoneum.
Arterial Supply
A. Blood supply to the cervical part is by inferior thyroid arteries.
B. Blood supply to the thoracic part is by esophageal branches of Descending thoracic aorta, and Bronchial arteries.
C. Blood supply to the abdominal part is by esophageal branches of Left gastric artery, and Left inferior phrenic artery.
Venous Drainage
A. Cervical part is drained by inferior thyroid veins.
B. Thoracic part is drained by azygos and hemiazygos veins.
C. Abdominal part is drained by 2 venous channels, viz,
- hemiazygos vein, a tributary of inferior vena cava, and
- left gastric vein, a tributary of portal vein.
Thus abdominal part of esophagus is the site of portocaval anastomosis.
Lymphatic Drainage
A. From cervical part, the lymph is drained into deep cervical lymph nodes.
B. From thoracic part, the lymph is drained into posterior mediastinal lymph nodes.
C. From abdominal part, the lymph is drained into left gastric lymph nodes.
Nerve Supply
The esophagus is supplied by both parasympathetic and sympathetic fibres.
The parasympathetic fibres are originated from recurrent laryngeal nerves and esophageal plexuses created by vagus nerves. They supply sensory, motor, and secretomotor supply to the esophagus.
The sympathetic fibres are originated from T5-T9 spinal segments are sensory and vasomotor.
Microscopic Structure
Histologically, esophageal tube from inside outwards is created from the following 4 basic layers:
Mucosa
It’s composed of the following components:.
A. Epithelium – highly stratified squamous and non- keratinized.
B. Lamina propria – contains cardiac esophageal glands in the lower part only.
C. Muscularis mucosa – very-very thick and created from only longitudinal layer of smooth muscle fibres.
Submucosa
It includes mucous esophageal glands.
Muscular Layer
A. In upper 1 -third, it’s created from skeletal muscle.
B. In middle 1 -third, it’s created from both skeletal and smooth muscles.
C. In lower 1 -third, it’s created from smooth muscle.
Fibrous Membrane (Adventitia)
It is composed of dense connective tissue that has many elastic fibres.
A clinical condition at which stratified squamous epithelium of esophagus is replaced by the gastric epithelium is referred to as Barrett esophagus. It may result in esophageal carcinoma.
Development Of The Esophagus And Trachea
The esophagus develops from foregut. The respiratory tract develops from foregut diverticulum referred to as laryngotracheal diverticulum/tube. The following 2 essential events happen in the development of esophagus:
- Separation of laryngotracheal tube by the formation of laryngotracheal septum.
- Recanalization of obliterated lumen.
The failure of canalization of the esophagus leads to esophageal atresia and maldevelopment of laryngotracheal septum between the esophagus and trachea leads to tracheoesophageal fistula.
Clinical Significance
Cervical Part of Esophagus
The left margin of the esophagus projects laterally from behind the trachea in the region of the neck. Thus the cervical part of esophagus can be marshalled and exposed surgically more easily from the left side.
The inner part of the esophagus can be examined in vivo by esophagoscope. This process helps to get tissue biopsy or removal of swallowed foreign body.
Esophageal Varices
The lower end of esophagus is 1 of the significant sites of portocaval anastomosis. In portal hypertension, example, because of the cirrhosis of liver there’s back pressure in portal circulation. Because of this, collateral channels of portocaval anastomosis not only open up but become dilated and tortuous to create esophageal varices. The ruptured esophageal varices cause hematemesis (vomiting of blood).
In the esophageal aperture of the diaphragm, the left vagus nerve (now referred to as anterior gastric nerve) is related anteriorly and right vagus nerve (now termed posterior gastric nerve) is related posteriorly.
Referred Pain Of Esophagus
The pain sensations mostly originates from the lower part of the esophagus as it’s susceptible to acid-peptic esophagitis. Pain sensations are carried by sympathetic fibre to the T4 and T5 spinal segments.
For that reason, esophageal pain is referred to the lower thoracic region and epigastric region of the abdomen, and at times it becomes difficult to differentiate esophageal pain from the anginal pain.
Clinical Importance Of Esophageal Constrictions
The anatomical constrictions of esophagus are of considerable clinical importance because of the following reasons:
- These are the sites where swallowed foreign bodies may stuck in the esophagus.
- These are the sites where strictures develop after ingestion of caustic substances.
- These sites have predilection for the carcinoma of the esophagus.
- These are sites via which it might be difficult to pass esophagoscope/gastric tube.
Radiological Evaluation Of The Esophagus By Barium Swallow
It’s performed to detect (a) enlargement of the left atrium because of mitral stenosis, (b) esophageal strictures, and (c) carcinoma and achalasia cardia.
In normal case, the barium swallow examination presents 3 indentations in its outline caused by the aortic arch, left principal bronchus, and left atrium.
Esophagoscopy
It’s performed to visualize the interior of the esophagus while passing esophagoscope, the sites of normal constrictions ought to be kept in mind.
Achalasia Cardia
It’s a clinical condition where sphincter at the lower end of esophagus fails to relax when the food is swallowed. Consequently food accumulates in the esophagus and its regurgitation takes place. This condition takes place because of neuromuscular incoordination, probably because of congenital absence of ganglion cells in the myenteric plexus of nerves in the esophageal wall. A radiographic barium swallow evaluation of the esophagus reveals a characteristic birds beak/rat tail appearance.
Dysphagia (Difficulty In Swallowing)
It takes place because of:
- Compression of esophagus from outside by aortic arch aneurysm, enlargement of lymph nodes, abnormal right subclavian artery (passing posterior to esophagus), etc. and
- Narrowing of lumen because of stricture or carcinoma.
Tracheoesophageal Fistula
It’s a commonest congenital anomaly of esophagus which takes place because of failure of separation of the lumen of tracheal tube from that of esophagus by a laryngotracheal septum. In the most commonest type of tracheoesophageal fistula, the upper esophagus ends blindly and lower esophagus interacts with trachea in the level of T4 vertebra. Medically it presents as: (a) hydramnios because fetus is unable to swallow amniotic fluid, (b) stomach is distended with air, and (c) infant vomit every feed given or may cough up bile. The fistula must be closed surgically to avoid passage of swallowed liquids into the lungs.
Malignant Tumors Of Esophagus
They most commonly take place in its lower one-third.
The lymph vessels from lower 1/3rd of the esophagus descend via the esophageal opening of the diaphragm and drain into the celiac lymph nodes around the celiac trunk. A malignant tumor from lower 1/3rd of esophagus, for that reason, spreads below the diaphragm into these lymph nodes. Consequently, surgical resection of the lesion consists of not only the primary site (i.e., esophagus) but also celiac lymph nodes and all the regions that drain into these lymph nodes like stomach, upper half of the duodenum, spleen, and omenta. The continuity of gut is restored by performing an esophagojejunostomy.
Test Your Knowledge
oesophagus

 (55 votes, average: 4.55 out of 5)
(55 votes, average: 4.55 out of 5)