Vagina is a female organ of copulation, comprising of the lower part of the beginning canal. The meaning of the term vagina is sheath (cf. vagina creates sheath around the penis during copulation).
Synonym: Greek Kolpos: vagina; use of terms like colpotomy and colporrhaphy.
From the vestibule of the vagina (a cleft between the labia minora) to the uterus, it goes both upwards and backwards. It is situated between the bladder and urethra in front and rectum and the anal canal behind.
The axis of the vagina corresponds with the axis of the pelvic outlet.
Size And Shape
Length: The anterior wall of the vagina is 7.5 cm in length, while on the other hand, the posterior wall is 9 cm long.
Width: It slowly rises from below upward. The diameter of the upper end is approximately double in size to that at the lower end.
- The diameter of the upper end: 5 cm.
- Diameter at the lower end: 2.5 cm.
The lumen of the vagina in cross section:
- In the lower one-third: H-shaped.
- In the middle one-third: Transverse slit.
- In the upper one-third: Round/circular.
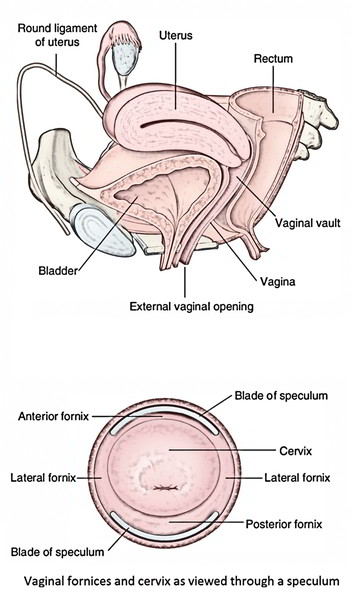
Fornices of Vagina
The upper part of the vagina encircles the cervix of the uterus. The circular area of vaginal lumen around the cervix is named fornix of the vagina. It’s a short distance above the external os, and deep behind than in front. For the sake of description, the fornix of the vagina is split into 4 parts:
- Anterior part/anterior fornix.
- Posterior part/posterior fornix.
- 2 lateral parts/lateral fornices.
The posterior fornix is all about 2 cm deeper in relation to the anterior fornix.
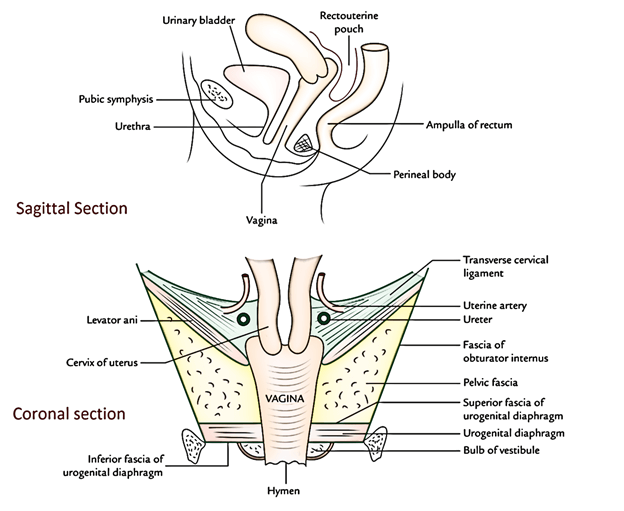
Relationships
Anteriorly
- The upper half is associated with the base of the urinary bladder.
- The lower half is related to the urethra that is truly embedded in it.
Posteriorly
- The upper quarter is associated with the rectouterine pouch (or pouch of Douglas).
- The middle two-fourth is linked to the ampulla of the rectum from which it’s divided by loose connective tissue.
- The lower quarter is associated with the perineal body dividing it from the anal canal.
Laterally
- The upper part is associated with the ureters that are close to the lateral fornices and are crossed by the uterine artery.
- The middle part is associated with the anterior fibres of levator ani (pubococcygeus part) and pelvic fascia.
- The lower part is related to the urogenital diaphragm, bulb of vestibule, bulbospongiosus, and greater vestibular gland (of Bartholin).
Structure
The wall of vagina includes the following 3 layers:
- An outer adventitial layer is composed of loose connective tissue. It includes blood vessels, lymphatics, and nerves.
- A muscular layer is created from smooth muscle which is composed of an outer longitudinal layer and inner circular layer.
- Mucous lining:
- The epithelium is stratified, squamous, non-keratinized including glycogen in adult women.
The fluid in the vagina is kept acidic by fermentive activity of particular bacteria (Doderleins bacilli) on glycogen, creating lactic acid.
- Lamina propria is dense and includes many elastic fibres.
There are not any glands in the vaginal mucous membrane, but it’s kept damp or lubricated by mucous originated from the glands of cervix.
The combo of muscular layer and an extremely elastic lamina propria enables the gross distension of the vagina during parturition (childbirth).
Hymen of Vagina
- It’s an incomplete mucous fold shutting the vaginal cavity near the external orifice of the vagina. The hymen presents different contours- annular, crescentic, or cribriform. During coitus the hymen ruptures and becomes fissured creating license plates of mucous membrane named caruncles.
- Scarcely the hymen is an entire membrane and obstructs discharge of the blood during menstruation leading to hematocolpos.
- The features of hymen are analyzed for the medicolegal function to verify virginity.
Arterial Supply
The vagina is a very vascular organ and is supplied by the following arteries:
- Vaginal artery, a branch of the internal iliac artery (principal artery).
- Vaginal branch of uterine artery.
- Internal pudendal artery.
- Middle rectal artery.
- Inferior vesical artery.
The vaginal branches of uterine internal iliac arteries anastomose to create midline longitudinal vessels (azygos vaginal arteries) along the anterior and posterior vaginal walls.
Venous Drainage
The veins of the vagina create a rich venous plexus referred to as pampiniform plexus in the sides of vagina which empties via vaginal veins into the internal iliac veins.
Lymphatic Drainage
The lymphatics of vagina are split into 3 groups:
- From upper one-third of the vagina, lymphatics accompany the uterine artery to drain into internal and external iliac nodes.
- From middle one-third of the vagina, lymphatics accompany the vaginal artery to drain into internal iliac nodes.
- From lower one-third, (strictly speaking vagina below the hymen) of lymphatics accompany those from the vulva to drain into the medial group of superficial inguinal nodes.
Nerve Supply
- The upper two-third of the vagina is insensitive to pain, touch, and temperature but it’s sensitive to extend. It’s supplied by the sympathetic (L1, L2 spinal sections) and parasympathetic (S2, S3 spinal sections) fibres.
- The lower one-third of vagina, consisting of region of vaginal orifice, is exceptionally sensitive to touch. It’s supplied by the pudendal nerve via inferior rectal and posterior labial branches of perineal nerve.
Clinical Significance
Per vaginal (PV) evaluation is carried out to estimate the distinct pathological circumstances by palpating the pelvic organs.
Vaginitis
Vaginitis (infection of vagina) is unusual in healthy adult females as the vagina is self-sterilizing in mature owing to its acidic medium (pH = 4.5) where organisms are unable to grow. In the child, the normal defence mechanism of the vagina is absent.
The acidic medium is because of the presence of Doderlein’s bacilli creating lactic acid from glycogen in the vaginal epithelial cells that is dependent upon the action of estrogen on the cells causing development and maturation. After menopause the vaginal epithelium atrophies. For that reason, vaginitis is common in kids and old women (after menopause).
Prolapse
The prolapse of anterior vaginal wall may drag the urinary bladder (cystocele) or urethra (urethrocele). The prolapse of the posterior vaginal wall drags the rectum (rectocele).
Culdocentesis
It’s a clinical process where a needle is gone through the posterior fornix of vagina into the rectouterine pouch (of Douglas) to drain the pus collected in this pouch in pelvic inflammatory disease or blood following rupture of the fallopian tube because of ectopic tubal pregnancy. Now this process is utilized to acquire a fluid sample for gathering oocytes for in vitro fertilization.

 (63 votes, average: 4.81 out of 5)
(63 votes, average: 4.81 out of 5)