Epithelial tissues, or epithelia (singular, epithelium), may be composed of one or more layers of cells. The number of cell layers and the shape of the cells provide the basis for classifying epithelial tissues. Epithelial tissues are distinguished by the following five characteristics:
- Epithelial cells are packed closely together with very little extracellular material between them.
- The sheetlike tissue is firmly attached to the deeper connective tissue by a thin layer of proteins and carbohydrates called the basement membrane.
- The surface of the tissue (free surface) opposite the basement membrane is not attached to any other type of tissue and is located on a surface or next to an opening.
- Blood vessels are absent, so epithelial cells must rely on diffusion to receive nourishment from blood vessels in the deeper connective tissue. Because these tissues are on surfaces, they are prone to damage. The lack of blood vessels prevents unnecessary bleeding.
- Epithelial tissues regenerate rapidly by mitotic cell division of the cells. Large numbers of epithelial cells are destroyed and replaced each day.
The functions of epithelial tissues vary with the specific location and type of tissue, but generally, they include protection, diffusion, osmosis, absorption, filtration, and secretion. Certain epithelial cells form glandular epithelium, the cells in glands that produce secretions. Two basic types of glands are contained in the body: exocrine and endocrine glands. Exocrine glands (exo = outside of; crin = to secrete) have ducts (small tubes) that carry their secretions to specific areas; sweat glands and salivary glands are examples. Endocrine glands (endo = within) lack ducts. Their secretions, called hormones, are carried by the blood supply to organs within the body to regulate their function. The thyroid gland and adrenal glands are examples of endocrine glands.
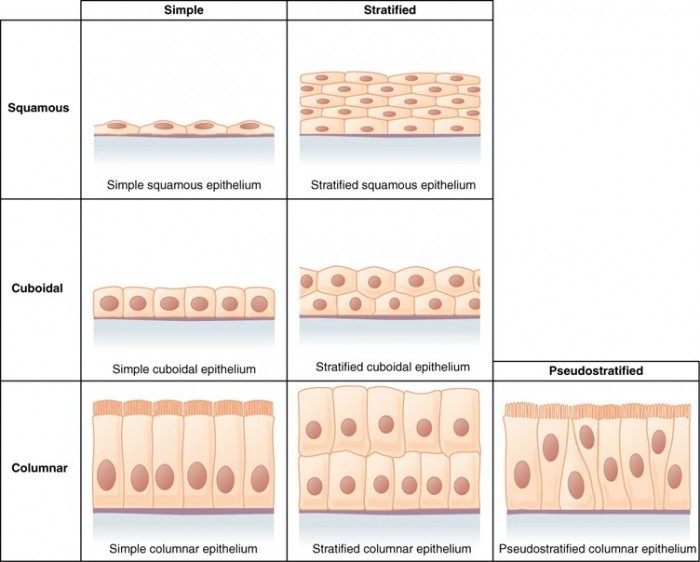
Simple Epithelium
Generally, a simple epithelium has only one layer of cells, although this is a somewhat debatable point in the pseudostratified type. Three types of simple epithelia are named for the shapes of their cells: simple squamous (thin scaly cells), simple cuboidal (square or round cells), and simple columnar (tall narrow cells). In the fourth type, pseudostratified columnar, not all cells reach the free surface; the shorter cells are covered over by the taller ones. This epithelium looks stratified in most tissue sections, but a careful examination, especially with the electron microscope, shows that every cell reaches the basement membrane—like trees in a forest all anchored in the soil, but with some growing taller than others. Simple columnar and pseudostratified columnar epithelia often produce protective mucous coatings over the mucous membranes. The mucus is secreted by wineglass-shaped goblet cells.
Simple Squamous Epithelium
Simple epithelium consists of a single layer of cells that may be flat (squamous), cube-like (cuboidal), and column-like (columnar) in shape. These tissues are located where rapid diffusion, secretion, or filtration occur in the body. Simple squamous (skwa’-mus) epithelium consists of thin, flat cells that have an irregular outline and a flat, centrally located nucleus. In a surface view, the cells somewhat resemble tiles arranged in a mosaic pattern. Simple squamous epithelium performs a diverse set of functions that include diffusion, osmosis, filtration, secretion, absorption, and friction reduction. Its locations in the body include
(1) The air sacs in the lungs, where O2 and CO2 diffuse into and out of the blood, respectively;
(2) Special structures in the kidney called glomeruli (glo-mer’u-li), where blood is filtered during urine production;
(3) The mesothelium, which is part of the serous membranes lining the ventral cavity;
(4) and the endothelium, which lines the internal surfaces of the heart, blood vessels, and lymphatic vessels.
Microscopic appearance: Single layer of thin cells, shaped like fried eggs with bulge where nucleus is located; nucleus flattened in the plane of the cell, like an egg yolk; cytoplasm may be so thin it is hard to see in tissue sections; in surface view, cells have angular contours and nuclei appear round
Representative locations: Air sacs (alveoli) of lungs; glomerular capsules of kidneys; some kidney tubules; inner lining (endothelium) of heart and blood vessels; serous membranes of stomach, intestines, and some other viscera; surface mesothelium of pleura, pericardium, peritoneum, and mesenteries
Functions: Allows rapid diffusion or transport of substances through membrane; secretes lubricating serous fluid
Simple Cuboidal Epithelium
Simple cuboidal epithelium consists of a single layer of cube-shaped cells. The cells have a single, round, centrally located nucleus. Its basic functions are absorption and secretion. Locations for simple cuboidal epithelia include (1) the secretory portion of glands, such as the thyroid and salivary glands; (2) the kidney tubules where secretion and reabsorption of materials occur; and (3) the superficial layer of the ovaries.
Microscopic appearance: Single layer of square or round cells; in glands, cells often pyramidal and arranged like segments of an orange around a central space; spherical, centrally placed nuclei; with a brush border of microvilli in some kidney tubules; ciliated in bronchioles of the lung.
Representative locations: Liver, thyroid, mammary, salivary, and other glands; most kidney tubules; bronchioles.
Functions: Absorption and secretion; production of the protective mucous coat; movement of respiratory mucus.
Simple Columnar Epithelium
Simple columnar epithelium consists of a single layer of elongated, columnar cells with oval nuclei usually located near the basement membrane. Scattered among the columnar cells are goblet cells, specialized mucus- secreting cells with a goblet or wine glass shape. Their purpose is to secrete a protective layer of mucus on the free surface of the epithelium. Secretion and absorption are the major functions of this tissue in areas such as the stomach and intestines. The cells lining the intestine possess numerous microvilli on their free surface, often called a “brush border” because of its bristle-like appearance, which greatly increases their absorptive surface area. In areas such as uterine tubes, paranasal sinuses, and ventricles of the brain, this tissue possesses cilia that allow for movement of materials across the tissue surface.
Microscopic appearance: Single layer of tall, narrow cells; oval or sausage-shaped nuclei, vertically oriented, usually in basal half of cell; apical portion of cell often shows secretory vesicles visible with TEM; often shows a brush border of microvilli; ciliated in some organs; may possess goblet cells
Representative locations: Inner lining of stomach, intestines, gallbladder, uterus, and uterine tubes; some kidney tubules
Functions: Absorption; secretion of mucus and other products; movement of egg and embryo in uterine tube
Pseudostratified Ciliated Columnar Epithelium
Pseudostratified ciliated columnar epithelium consists of a single layer of cells. It is said to be pseudostratified (pseudo = false) because its structure creates a visual illusion of being multilayered but it really is a simple epithelium. The layered effect results in part from the nuclei being located at various levels within the cells. Also, even though all of the cells are attached to the basement membrane, not all of them reach the free surface. Just as in simple columnar epithelium, goblet cells are scattered throughout the tissue. This epithelium lines the internal surfaces of many of the respiratory passageways, where it collects and removes airborne particles. The particles are trapped in the secreted mucus, which is moved by the beating cilia to the throat, where it is either swallowed or expectorated.
Microscopic appearance: Looks multilayered; some cells do not reach free surface, but all cells reach basement membrane; nuclei at several levels in deeper half of epithelium; often with goblet cells; often ciliated
Representative locations: Respiratory tract from nasal cavity to bronchi; portions of male urethra
Functions: Secretes and propels mucus
Stratified Epithelium
Stratified epithelia range from 2 to 20 or more layers of cells, with some cells resting directly on others and only the deepest layer attached to the basement membrane. Three of the stratified epithelia are named for the shapes of their surface cells: stratified squamous, stratified cuboidal, and stratified columnar epithelia. The deeper cells, however, may be of a different shape than the surface cells. The fourth type, transitional epithelium, was named when it was thought to represent a transitional stage between stratified squamous and stratified columnar epithelium. This is now known to be untrue, but the name has persisted.
Stratified columnar epithelium is rare—seen only in places where two other epithelial types meet, as in limited regions of the pharynx, larynx, anal canal, and male urethra. We will not consider this type any further.
The most widespread epithelium in the body is stratified squamous epithelium, which deserves further discussion. Its deepest layer of cells is cuboidal to columnar stem cells, which undergo continual mitosis. Their daughter cells push toward the surface and become flatter (more squamous, or scalelike) as they migrate farther upward until they finally die and flake off. Their separation from the surface is called exfoliation, or desquamation; the study of exfoliated cells is called exfoliate cytology. You can easily study exfoliated cells by scraping your gums with a toothpick, smearing this material on a slide, and staining it. A similar procedure is used in the Pap smear, an examination of exfoliated cells from the cervix for signs of uterine cancer.
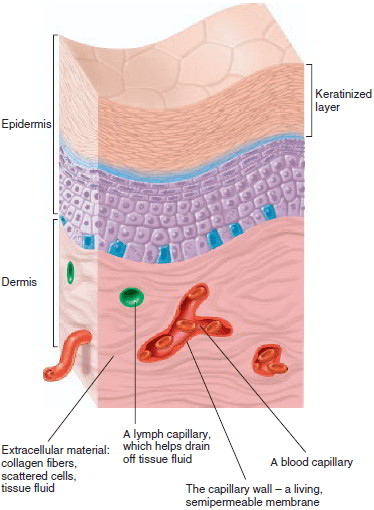
Stratified squamous epithelia are of two kinds: keratinized and nonkeratinized. A keratinized epithelium, found on the skin surface (epidermis), is covered with a layer of compact, dead squamous cells. These cells are packed with the durable protein keratin and coated with a water repellent glycolipid. The skin surface is therefore relatively dry, it retards water loss from the body, and it resists penetration by disease organisms. (Keratin is also the protein of which animal horns are made, hence its name.) The tongue, esophagus, vagina and a few other internal membranes are covered with the nonkeratinized type, which lacks the surface layer of dead cells. This type provides a surface that is, again, abrasion-resistant, but also moist and slippery. These characteristics are well suited to resist stress produced by the chewing and swallowing of food and by sexual intercourse and childbirth.
Stratified Squamous Epithelium
Stratified squamous epithelium occurs in two distinct forms: keratinized and nonkeratinized. The keratinized type forms the superficial layer (epidermis) of the skin. Its cells become impregnated with a waterproofing protein, keratin (ker’-ah-tin), as they migrate to the free surface of the tissue. The nonkeratinized type lines the mouth, esophagus, vagina, and rectum. Both types provide resistance to abrasion.
Stratified Squamous Epithelium-Keratinized
Microscopic appearance: Multiple cell layers with cells becoming increasingly flat and scaly toward surface; surface covered with a layer of compact dead cells without nuclei; basal cells may be cuboidal to columnar
Representative locations: Epidermis; palms and soles are especially heavily keratinized
Functions: Resists abrasion; retards water loss through skin; resists penetration by pathogenic organisms
Stratified Squamous Epithelium—Nonkeratinized
Microscopic appearance: Same as keratinized epithelium but without the surface layer of dead cells
Representative locations: Tongue, oral mucosa, esophagus, anal canal, vagina
Functions: Resists abrasion and penetration by pathogenic organisms
Stratified Cuboidal Epithelium
Microscopic appearance: Two or more layers of cells; surface cells square or round
Representative locations: Sweat gland ducts; egg-producing vesicles (follicles) of ovaries; sperm-producing ducts (seminiferous tubules) of testis
Functions: Contributes to sweat secretion; secretes ovarian hormones; produces sperm
Transitional Epithelium
Transitional epithelium lines most of the urinary tract and stretches as these structures fill with urine. It consists of multiple layers of cells, with the free surface cells of the unstretched tissue possessing a large and rounded shape. When stretched, the free surface cells become thin, flat cells resembling squamous epithelial cells.
Microscopic appearance: Somewhat resembles stratified squamous epithelium, but surface cells are rounded, not flattened, and often bulge at surface; typically five or six cells thick when relaxed and two or three cells thick when stretched; cells may be flatter and thinner when epithelium is stretched (as in a distended bladder); some cells have two nuclei
Representative locations: Urinary tract part of kidney, ureter, bladder, part of urethra; allantoic duct in umbilical cord
Functions: Stretches to allow filling of urinary tract
Epithelial Membranes
Membranes of the body are thin sheets of tissue that line cavities, cover surfaces, or separate tissues or organs. Some are composed of both epithelial and connective tissues; others consist of connective tissue only.
Sheets of epithelial tissue overlying a thin supporting framework of areolar connective tissue form the epithelial membranes in the body. Blood vessels in the connective tissue serve both connective and epithelial tissues. There are three types of epithelial membranes: serous, mucous, and cutaneous membranes (figure 4.24).
Serous membranes, or serosae, line the ventral body cavity and cover most of the internal organs. They secrete serous fluid, a watery fluid, which reduces friction between the membranes. The pleurae, pericardium, and peritoneum are serous membranes. Recall that the epithelium of a serous membrane is a special tissue called mesothelium.
Mucous membranes, or mucosae, line tubes or cavities of organ systems, which have openings to the external environment. Their goblet cells secrete mucus, which coats the surface of the membranes to keep the cells moist and to lubricate their surfaces. The mucus also helps to trap foreign particles and pathogens, which limits their ability to enter the body. The digestive, respiratory, reproductive, and urinary tracts are lined with mucous membranes.
The cutaneous membrane is the skin that covers the body. Unlike other membranes, its free surface is dry, composed of nonliving cells, and exposed to the external environment.
Connective Tissue Membranes
Some specialized membranes are formed only of connective tissue, usually dense irregular connective tissue. Here are four examples:
- The meninges are three connective tissue membranes that envelop the brain and spinal cord.
- The perichondrium is a connective tissue membrane covering the surfaces of cartilage. It contains blood vessels, which supply cartilage through diffusion.
- The periosteum is a connective tissue membrane that covers the surfaces of bones. It contains blood vessels that enter and supply the bone.
4. Synovial membranes line the cavities of freely movable joints, such as the knee joint. They secrete watery synovial fluid, which reduces friction in the joint.

 (48 votes, average: 4.58 out of 5)
(48 votes, average: 4.58 out of 5)