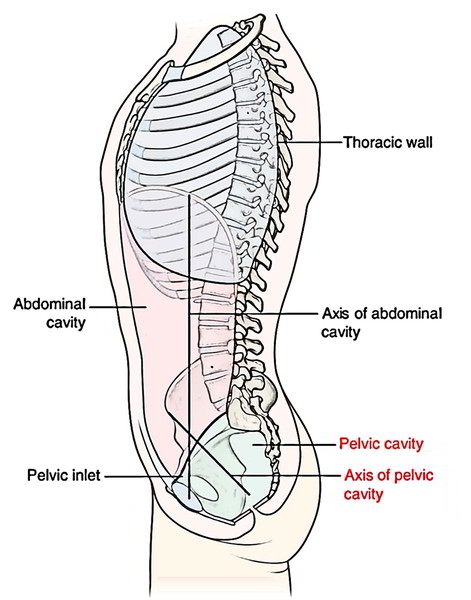
The shape of pelvic cavity is much similar to that of funnel. Peritoneum continuous with the peritoneum of the abdominal cavity lines the pelvic cavity that drapes over the superior aspects of the pelvic viscera, but does not reach the pelvic floor in the majority of the regions.
The pelvic viscera are located in the midline of the pelvic cavity. The bladder is anterior and the rectum is posterior. In women, the uterus lies between the bladder and rectum. Other structures, such as vessels and nerves, lie deep to the peritoneum in association with the pelvic walls and on either side of the pelvic viscera.
Its borders and contents are as follows:
Borders
The borders of the pelvic cavity are:
- Superiorly: Constant with the abdominal cavity in the pelvic inlet.
- Inferiorly: Pelvic diaphragm.
- Posteriorly: Sacrum and coccyx.
- Anteriorly: Pubic bones.
- Laterally: Hip bones.
The part of pelvis below the pelvic diaphragm is called perineum.
Contents
The pelvic cavity includes these structures:
- Loops of the small intestine.
- Sigmoid colon, rectum, and anal canal.
- Urinary bladder, lower part of the ureters, and urethra.
- Reproductive organs:
a) Prostate gland, seminal vesicles, vas deferens, and ejaculatory ducts in male.
b) Uterus, uterine tubes, ovaries, and vagina in female.
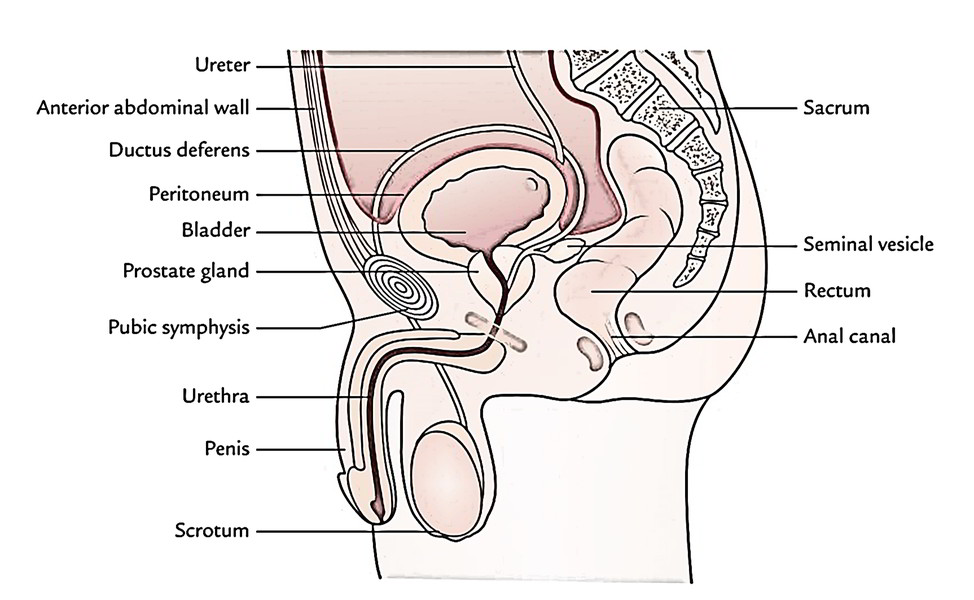
Male
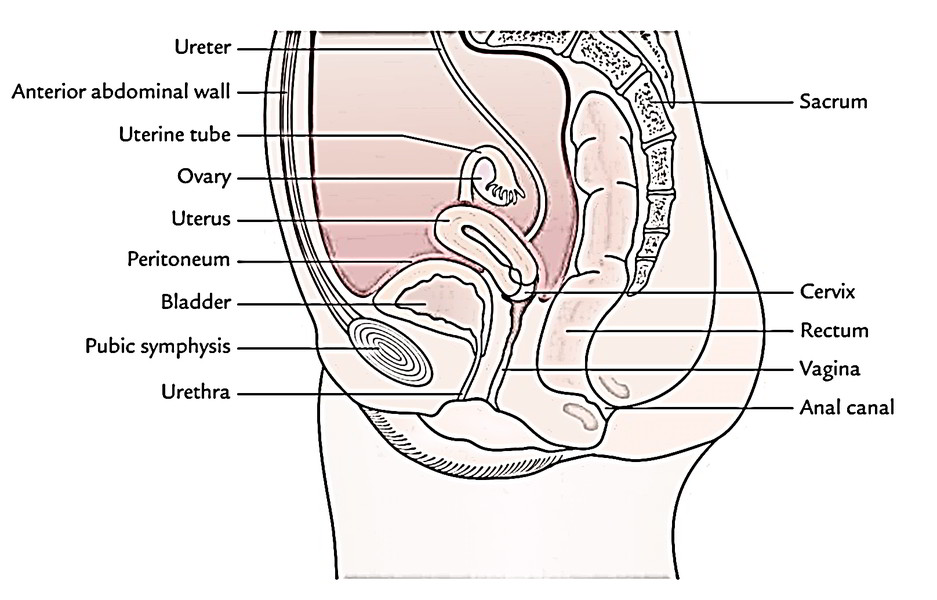
Female
The Pelvic Cavity is the cavity in which all the organs, muscles, nerves, blood vessels and other structures are housed. The pelvic and urogenital diaphragms creating the inferior boundary of the pelvic cavity support the pelvic viscera and modulate the action of defecation, micturition, and parturition.
The walls of the abdominal cavity and majority of the viscera present inside it are covered or enclosed by an extensive serous membrane referred to as peritoneum. The peritoneum is made of parietal and visceral layers, which are constant with every other and enclose a potential space named peritoneal cavity.
Points to be noticed
- All the abdominal viscera are intra-abdominal but extraperitoneal with the exception of the ovaries in female.
- The peritoneal cavity is a closed sac in the male however in the female it’s an open sac and interacts to the outside via the openings of the uterine tubes.
Pelvic Viscera
The pelvic viscera in males are urinary bladder, prostate, and rectum; and in females are urinary bladder, uterus, and rectum
Urinary Bladder
The urinary bladder is a reservoir of pee. Its size, shape, and position change together with the amount of urine it includes. When empty it is located in the pelvic cavity, but when distended with urine it grows upward and forward into the abdominal cavity. The bladder can hold up to 500 ml (infrequently 600 ml) of urine, though this would cause pain. The want to empty the bladder is normally felt when it includes around 250-300 ml of urine.
The 2 ureters goes into it via its posterior wall. The urethra makes the bladder at its neck. The neck of the bladder is the lowest and most fixed part of the urinary bladder. A thickening of smooth muscle termed internal urethral sphincter encompasses the opening of the urethra.
Function
The urinary bladder stores urine and expels it into the urethra.
Urethra
The urethra is a narrow canal that goes from the internal urethral orifice in the urinary bladder to the external urethral orifice.
In a male, the urethra is all about 18-20 cm long and in a female, it’s about 4 cm long.
Functions
In a male, the urethra acts as a common passage for both semen and urine on the other hand in a female, the urethra discharges urine from the body.
Prostate Gland
The prostate is a fibromusculoglandular organ, which encompasses the commencement of the urethra in the male. It’s situated in the pelvic cavity behind the pubic symphysis and in front of the rectum. It’s about the magnitude of a chestnut and is traversed by the urethra and ejaculatory ducts.
Function
The function of the prostate is really to secrete a thin, milky fluid, which creates about 30% of the semen, and provides it a milky look. The prostatic secretion is alkaline in nature and gives nourishment to the sperms.
Seminal Vesicles
The seminal vesicles are just two small fibromuscular pouches being located between the base of the bladder and the rectum.
Function
The seminal vesicles secrete an alkaline fluid consisting of nutrients for the sperms and creates about 60% of the seminal fluid.
Ejaculatory Ducts
The ejaculatory ducts are 2 narrow tubes about 1 cm long. The duct of seminal vesicle and ductus deferens unify to create ejaculatory duct. They traverse the prostate gland to open into the urethra inside the gland (prostatic part of urethra).
Function
The ejaculatory ducts expel the secretions of testes and seminal vesicles into the prostatic urethra.
Uterus
The uterus is a hollow, thick-walled, muscular organ situated in the pelvic cavity between the urinary bladder and the rectum. It’s pear shaped and flattened anteroposteriorly. In most women it leans forwards (anteflexion) andbends forwards (variant) nearly at a right angle to the vagina. In the erect bearing, the uterus is located in a just about horizontal position.
The uterus is split from above downward into following 3 parts: (a) fundus, (b) body, and (c) cervix. The cervix protrudes into the vagina via its anterior wall and opens into it at the external os.
Above on either side, it interacts with all the uterine tubes, which open into it. Below it interacts with the vagina.
Functions
The functions of the uterus after puberty are:
- Responsible for menstrual cycle (MC).
- Gives implantation to zygote in its wall.
- Enables growing and development of the embryo and fetus.
Vagina
The vagina is a fibromuscular tube, which extends obliquely downward and forward from the uterus to the vestibule of vagina- the elliptical space between the labia. It’s situated between the urinary bladder in front, and the rectum and anal canal behind. The vagina has no secretory glands though it’s kept damp by the cervical secretions.
Functions
The functions of the vagina are as follows:
- Actions as a receptacle for penis during coitus.
- Gives an elastic passage to the baby during childbirth.
Uterine Tubes
There are just two uterine tubes. Every tube is all about 10 cm long, which stretches from the side of the uterus (between the fundus and body) to the ovary where it opens into the peritoneal cavity.
It’s split into the following parts from distal to the proximal end: (a) infundibulum, (b) ampulla, (c) isthmus, and (d) intramural.
Functions
The functions of uterine tubes are as follows:
- Carry the ovum from ovary to its lumen and gives a perfect site for fertilization.
- Carry the fertilized ovum to uterine cavity for implantation.
Ovaries
The ovaries are female gonads. Every ovary is all about the size and shape of an almond and is situated in a shallow fossa onthe lateral wall of the pelvic cavity behind and below the distal end of the uterine tube.
Functions
The ovaries start to work at puberty and keep to release ova at monthly intervals from regarding the age of 13 years to concerning the age of 45 years.
Clinical Significance
- The upper part of the abdominal cavity is overlapped by the lower thoracic region and the lower part by the gluteal region. For that reason, the penetrating wounds of these regions often demand the abdominal viscera also.
- The upper abdominal contents like liver and spleen fill the concavity of the diaphragm. For that reason, it’s simple for the surgeons to reach these organs via the thorax and diaphragm or via the anterior abdominal wall.
- The mobile diaphragm creates the upper boundary/limit of the abdominal cavity; the abdominal contents descend with it on deep inspiration. This is made use of in clinical examination of particular organs, like liver and enlarged spleen, which can be palpated via the anterior abdominal wall, inferior to the costal margin on deep inspiration, though concealed by the thoracic cage in quiet respiration.
Disorders of the Abdomen
The disorders of the abdomen and pelvis are numerous; the significant ones are as follows:
Hernia
It’s the protrusion of an organ via the wall, which includes/ keeps it. The common abdominal hernias are inguinal, umbilical, femoral, and incisional; the order representing their frequency.
Abdominal Pain
Many intra-abdominal diseases present with pain only. The 2 essential features of an abdominal pain are its site and its nature. If a clinician understands about these features, he/ she’s a great opportunity of making a correct diagnosis. In general: (i) The upper abdominal pain mainly takes place because of engagement of gallbladder, stomach, duodenum, and pancreas. (ii) The central abdominal pain typically happens because of engagement of small bowel and kidneys. (iii) The lower abdominal pain takes place because of participation of urinary bladder, uterus, caecum, and sigmoid colon.

 (60 votes, average: 4.51 out of 5)
(60 votes, average: 4.51 out of 5)